Running can be tough in the best of times, but when the pain keeps getting worse until you cannot run another step, well, that is heartbreaking.
If you feel like the pain is coming from anywhere along the muscle on the outside of your thigh from your hip all the way down to your knee, you are not the only one, but it is actually not even a muscle at all.
Let us explain:
Your IT band injury (iliotibial band if you want to get technical) is probably stopping you, and as much as we wish we could tell you that this is an injury where you can run through the pain, it is not, and if you ignore where it hurts, it will keep getting worse until you literally cannot run anymore.
Today we are going to share what causes IT band syndrome (so you can make sure you never have to go through this again), and how to treat IT band pain if you are in the middle of it.

What is Your IT Band? Does IT Band Syndrome Explain my Symptoms?
The iliotibial band, or IT band, is a long “band” of tissue that runs from the top of the hips down the outside of the thigh, crossing the outside of the knee and inserting at the very top of the tibia.
While many people envision the IT band (ITB) as an independent structure that can freely slide forwards and backwards relative to the rest of the leg, in reality, it is nothing more than a thickened strip of fascia, the connective tissue that encapsulates the muscles of the body.
The IT band serves as a connection between many of the major hip muscles and the knee.
Its main function during running seems to be stabilizing the knee during footstrike.
ITB syndrome is an injury to the ITB. It most commonly occurs on the outside of the knee or just above it, though it is not unheard of to get pain further up the ITB, even as far as the top of the femur.
ITB syndrome accounts for somewhere between 8 and 10% of all running injuries,1 and doesn’t seem to discriminate: both recreational runners and elites suffer from this injury.
Your IT band usually gets sore after a set distance into a run—you’ll feel okay for a mile or two, but the outside of your knee will start to ache, progressing from a dull stiffness to a sharp or burning pain. It will almost feel like there is friction in there.
It typically hurts worse when going down hills, and you may sometimes feel pain when sitting with your leg bent for a long time.
Any activity which brings the knee into 20-30 degrees of flexion can aggravate the ITB, as this is when the band itself gets squeezed against the femur the most.
What Causes IT Band Syndrome and How To Stop it?
Just before the IT band crosses the knee, it runs on top of a large knob on the femur called the lateral epicondyle.
The prevailing opinion for a long time was that the IT band slides back and forth across this bony knob, leading to the term “IT band friction syndrome.”
However, recent anatomic studies have shown that the cause is more likely compression—the IT band is squeezed against the bone, irritating an area rich in blood vessels and nerve endings between the two structures.2
Okay, thats enough technical details for now.
What increases the risk of ITBS?
While factors like old shoes, running on cambered road surfaces, and tight turns on indoor tracks have all been proposed as risk factors for ITBS, none of these have much scientific evidence to back them up.
However, a host of studies have connected hip abductor and external rotator muscle weakness with ITBS.
In a healthy and strong runner, these muscle groups keep the hip abducted and the knee externally rotated, which limits the strain on the IT band.3, 4, 5
But when these muscles are weakened, the hip adducts and the knee internally rotates after impact with the ground, crushing the IT band and the underlying sensitive tissue against the lateral femoral epicondyle.
Current theories hold that the nerve endings sandwiched between the IT band and the femur are supposed to send signals to the glute muscles to fire when the IT band is being compressed—of course, when these muscles are weak or dysfunctional, this protection mechanism fails.
Instead of the gluteus medius and the other main hip abductors firing, the TFL (tensor fascia lata) muscle fires, which puts even more strain on the IT band. 2
One more reason to build those glutes, and give yourself a strong, toned butt!
Your stride width may be causing a crossover gait, which will be significantly increasing your risk of developing ITBS.
Correct your crossover gait, and you may say goodbye to ITB pain forever!
How To Treat IT Band Pain
If only there was a quick fix.
Would make life nice and easy, but unfortunately, there is no such thing. The best way to treat your IT band pain is to fix your running form.
IT band syndrome is a classic biomechanical problem.
Muscular weakness and dysfunction causes a predictable and repeatable change in running mechanics, increasing strain on the IT band and causing injury.
What does that mean?
While the painful area is the outside of the knee, the real problem lies further up the leg.
While icing, stretching, and foam rolling (just don’t foam roll right on the IT band or you WILL make it worse!) all have their role, a biomechanical problem ultimately needs a biomechanical solution.
This is where hip strengthening exercises come in.
The best current research-approved protocol for ITBS was described in a 2000 paper by Michael Fredericson at Stanford University.4
His rather simple program consists of two stretches and two strength exercises.
The stretches are performed three times per day holding the stretch for 15 seconds each on both sides. The strength exercises start with one set of 15 repeats every day, building up to three sets of 30 over time.
The entire program lasts six weeks. Fredericson’s athletes avoided running during this six-week protocol, and 92% recovered completely.
RunnersConnect Insider Bonus
Download our free Top 5 IT Band Prevention Exercises guide.
It’s a PDF with the 5 best exercises to help you prevent IT band syndrome.
The Fredericson protocol:
Lying rope hip stretch
Standing hip crossover stretch
Lying hip abduction
Standing hip hike
What Else Can Treat an IT Band Injury?
While Fredericson’s results were impressive, his study had some flaws.
For one, it had no control group, so it’s unclear how much of the improvement was from the exercises and how much was from the time off.
Additionally, his protocol lacks any exercises that strengthen the external rotators.
What’s the bottom line?
I recommend adding the following exercises to address external rotator and abductor strength at the same time, as well as adding some isometric strength, which is more similar to how these muscles function while running:
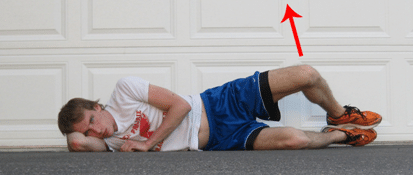
Clamshells
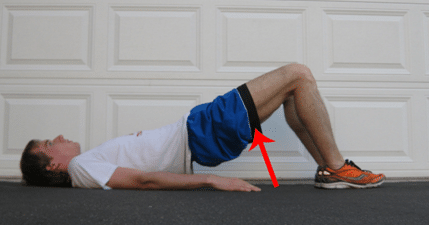
Glute bridge
The “up” position is held for 5 seconds
Wall isometric
The inside leg is pushed into the wall for a 5-second hold.
How to Stretch the IT Band
Don’t!
With regards to stretching, the IT band itself will not be very happy with it for two reasons:
First, it is not a stretchy tissue. Its stiffness is more in line with a car tire than a rubber band.6
Second, stretches that purportedly target the IT band don’t actually stretch it very much, since it attaches to the femur at several places.7
Instead, research suggests that you should target the muscles that attach to the IT band: the gluteus maximus and the TFL.
Fredericton already showed you the best IT band stretch above.
Foam roller for the IT band
Using a foam roller to loosen up soft tissue around the IT band is a great idea, but actually rolling over the painful area should be avoided.
Remember, IT band pain stems from irritating the highly sensitive area between the bony knob on the femur and the IT band, so you don’t want to further aggravate this spot!
Some people find that a particular shoe style aggravates their IT band, but there’s no scientific evidence that points towards any kind of shoe or custom insert causing or curing IT band problems.
All the evidence thus far points to the root cause being at the hips, not the feet, so your number one priority should be to strengthen your abductors and external rotators.
Summary of How to Treat IT Band Syndrome
Conservative treatments
These are methods that are fairly simple, inexpensive, and can be done on your own at home.
Hip strengthening: Fredericson protocol + added exercises:
Fredericson protocol:
- Lying hip stretch with rope
- Standing crossover stretch
- Lying hip abduction
- Standing hip hike
Additional exercises:
- Clamshell exercise, 1×15
- Glute bridge with 5sec hold
- Wall isometric with 5sec hold
Additional therapies:
- Foam rolling of the quads, hamstrings, glutes, and upper hip area 1-2x per day
- Icing with ice cup: 10-12 minutes, 2-5 times per day
Aggressive treatments
These are treatments with more cost and less certainty about outcomes, but may prove useful in recalcitrant cases.
Active Release Technique (ART) and/or Graston technique is probably your best bet to treating ITB pain.
These are soft tissue manipulation therapies that are intended to break down scar tissue in chronically injured areas.
While there is little to no science backing their efficacy, some runners have found relief from ART or Graston. Most practitioners are chiropractors, so this treatment may or may not be covered by insurance.
But, keep this in mind:
It should not be used immediately after hurting your IT band in an isolated incident.
Cross Training While Injured and During Recovery
Cross training is recommended while you’re injured and as you slowly return to running.
The best form of cross training for this injury is Aqua Jogging. Studies have shown that aqua jogging can enable a well-trained runner to maintain running fitness for up to 4-6 weeks.
Aqua jogging is a form of deep water running that closely mimics the actual running movement. Your feet don’t actually touch the bottom of the pool, so it is zero impact and safe for almost any type of injury. In my experience, the only time to avoid aqua jogging is when you have a hip flexor injury, which can be aggravated by the increased resistance of the water as you bring your leg up.
Because aqua jogging closely mimics natural running form, it provides a neuromuscular workout that, in addition to aerobic benefits, helps keep the running specific muscles active. The same can’t be said for biking and swimming.
The only downside to aqua jogging is that you need a pool that is deep enough to run in without touching the bottom. If you’re lucky enough to have access to a pool of this size, aqua jogging should be your first cross training choice.
In one study, a group of ten runners trained exclusively with deep water running for four weeks and compared 5km race times pre deep water running and post deep water running.
The researchers found no statistical difference in 5k time or other markers for performance, such as submaximal oxygen consumption or lactate threshold.
In a second study, researchers measured the effects of aqua jogging over a six week period.
This time, 16 runners were separated into two groups – one who did aqua jogging workouts and the other who did over land running.
Using the same training intensities and durations, the researchers found no difference between the groups in maximal blood glucose, blood lactate, and body composition.
It get’s better:
Research has also demonstrated that aqua jogging can be used as a recovery tool to facilitate the repair of damaged muscles after hard workouts.
These findings make aqua jogging an important recovery tool in addition to being the best cross training method for injuries.
Need one more reason?
The calories burned aqua jogging are even higher than running on land, so if you want to avoid weight gain while you take time off from running, this is definitely the exercise for you!
Aqua Jogging Workouts For Runners
If you’re interested in aqua jogging to rehab your injury, then the absolute best way is to use one of my favorite programs, Fluid Running.
First, it comes with an aqua jogging belt and waterpoof bluetooth headphones so you have everything you need to aqua jog effectively.
Second, they have an app that pairs with the headphones so you can get workouts, guided instructions on how to aqua jog properly, and motivation while you’re actually pool running.
This has been an absolute game changer for me when I am injured.
I used to dread aqua jogging workouts because they were so boring and it took all my mental energy to stay consistent.
But, with workouts directly in my ear, it’s changed the whole experience and I actually look forward to the workouts. So much so that I now use aqua jogging as a cross training activity in the summer, even when I am not injured.
Fluid running is an awesome deal when you consider it comes with the belt (highly recommended for better form), the waterproof headphones (game changer for making pool workouts fun), a tether (to add variety to the workouts you can do) and the guided workout app (to make your cross training structure and a whole lot more interesting).
That’s why we’ve partnered with them to give you 2 additional running-specific workouts you can load into the app when you use the code RTTT .
Check out the product here and then on the checkout page, add the code RTTT in the coupon field and the workouts will be added to your order for free.
If you’d rather do the aqua jogging workouts on your own, here are some great ideas to get you started!
Medium Effort Workouts
The Pyramid
10 minutes easy warm up – 1:00 hard, 30 seconds easy – 1:30 hard, 30 seconds easy – 2:00 hard, 30 seconds easy – 2:30 hard, 30 seconds easy, go to 5:00 in 30 second intervals and then come back down the pyramid (4:30 hard, 30 easy, 4:00 hard, 30 easy etc). Finish with 10 minutes easy cool down.
Wave your hands in the air like you just don’t care
10 minutes easy warm up, 1 minute medium (87-92% of maximum heart rate or what feels like tempo effort), 1 minute sprint (95-100% of maximum heart rate or all out sprint), 30 seconds hands in air (keep moving your legs in the running motion, but put your hand above your head), 1 minute rest, Repeat 10-15 times. 10 minutes easy cool down.
Hard Workouts
One of the difficulties of cross training is replicating those truly lung-busting, difficult workouts.
So, if you’re going to be pool running quite a bit due to injury or limited training volume, invest in a bungee cord designed for sprinters.
Tie one end of the resistance band to a sturdy object (pole, lifeguard stand, pool ladder) and bring the other into the water with you.
Put the strap around your waist and begin aqua jog away from your starting point.
You’ll begin to notice the bungee tighten and resist against you (depending on the length of your pool, you may need to wrap the bungee around the supporting object or tie it in knots to make it shorter to feel resistance).
Spend a few moments testing yourself to see how far you can pull the bungee.
This is a great challenge and a fun way to compete with yourself during an otherwise boring cross training activity.
Now for the hard part:
Pick a point on the pool wall or side of the pool that you feel stretches the bungee to a very hard sprint that you could maintain for 60-90 seconds.
This will be your “sprint” marker that you’ll use on sprint intervals (95-100% of maximum heart rate or all out sprint).
Now:
Find a point that feels like the end of a hard tempo run.
Mark this spot as your “medium” interval distance.
When you complete the hard workouts, you can use these reference points to ensure that you maintain a very hard effort.
The springboard
10 minutes easy warm up, 90 seconds easy (slowly moving out and stretching the bungee), 2 minute medium, 1 minute sprint, 1 min rest (let the bungee pull you back – this is kind of fun). Repeat 10 times. 10 minutes easy cool down.
The race simulation
10 minutes easy warm up, 90 seconds easy (slowly moving out and stretching the bungee), 5 minutes medium (focus and concentrate, just like during the hard part of a race), 30 seconds sprint, 2 minutes rest. Repeat 4 times. 10 minutes easy col down
The lactic acid
10 minutes easy warm up, 90 seconds easy (slowly moving out and stretching the bungee), 2 minutes sprint, 90 seconds rest. Repeat 12 times, 10 minutes easy cool down.
I guarantee that with the bungee, you’ll get your heart rate through the roof.
You can challenge yourself and make aqua jogging more fun by seeing how long you can stay at your maximum stretched distance or seeing how far you can push it.
Likewise, if you have a friend who is injured (or someone willing to be a good sport) you can try pulling each other across the pool for some competitive fun.
Cross training can be tough, especially when you’re injured or want to be increasing your volume faster.
However, I hope that providing a variety of workouts, either through the Fluid Running app (which also makes it easier to keep track of the workout while in the water) or on your own can add a fun challenge in the pool and you can emerge from your injury with minimal fitness loss.
How to Get Back to Running
Since IT band syndrome is the result of a biomechanical problem, your ability to return to running will be determined by your progress in hip strength.
In the initial stages of the injury, you will need anywhere from a few days to a few weeks of time off for the initial inflammation on the outside of the knee to calm down.
Icing often can speed this along.
Once the initial irritation is gone, you will probably find that your IT band still gets irritated after a few miles of running if you haven’t worked on your hip strength.
In my experience, it takes about a month of daily hip strength exercises to completely recover, though you may be able to run during this time period.
You just need to keep your runs short enough so that they do not aggravate your IT band anew.
If all else fails, you may need an extended break from running to rebuild your strength like the subjects in Fredericson’s study.
But don’t panic:
We have found that runners do not lose as much fitness as they think during time off running!
Phew!













38 Responses
Great article, down to earth and laid out in a good laymen’s terms that are easy to follow and understand (like most of your stuff) Thank you!
I’d add traditional sports/deep tissue massage as a great treatment, though I’m not sure I’d it as “aggressive” (seeing that massage is commonplace with runners) and the cost isn’t as high as ART or Graston, plus more accessible. A good practitioner knows how to handle the ITBand and surrounding muscles (hips, glutes, TFL, etc.) ART and Graston are great, pinpoint techniques and yes, more costly, but a good round of traditional sports massages have good success too in our experiences.
I’d also add Acupuncture to the more aggressive (and costly) list of Treatments. I’ve known many runners that have had luck, including my wife. After a debilitating bout of ITBS and 2-3 weeks of self and assisted care, 2 weeks of aggressive acupuncture did the trick (I’m sure the combination of everything helped) but it certainly stood out. (I’m a personal fan of acupuncture too and have seen it work well with many injuries and ailments.)
If I were to order the “practitioner assisted” treatments in relation to availability/cost/effectiveness/commonality, I’d do 1) Sports/Deep Massage 2) ART Massage 3) Graston 4) Acupuncture
Of course, the bigger picture is to get to the root causes like you point out so you don’t want to rely on massages every week, but getting through a bout of ITBS during training or leading to a race has to be dealt with, and sometimes very quickly.
Thanks, Blake. John really does a great job of breaking down the more complicated scientific findings into easily digestible and actionable findings.
I like both of your suggestions on massage and acupuncture. Actually, I think it would be beneficial to look at some of the science of these two modalities in more depth, rather than just on IT band injuries specifically. I think that could open up a valuable treatment method for some injuries.
Finally, you’re definitely right about finding the root cause. I think a lot of the hip exercises mentioned can really help address the structural weaknesses.
Thank you for the suggestions and ideas for future research. I appreciate the comment. Best of luck with your training and racing!
I agree with Blake regarding good old, traditional sports/deep tissue massage or just regular massage. I came across this article while looking for some stretching exercises for the IT band area. i have a client coming who has been told she has an IT band issue….. I will have to palpate and see if this is the case. At any rate, this article talks about the issues plainly – without too much medical jargon – and gives some great visuals on the stretching exercises. Am glad I bumped into this site.
I was actually going to ask about acupuncture as I have been reading about it as another treatment for IT band. I have been feeling like the stretching is not so helpful, but the hip/glute strengthening exercises are. I’m able to run up to 4 miles comfortably but have not gone beyond. I did take a couple weeks off completely but that really proved to be worse! As long as I can run without discomfort, I feel much better keeping a regular running schedule! Thanks for discussing this topic-very helpful!
I’ve been dealing with pain on the side of my left hip for months, and I can’t seem to get rid of it. In many ways it matches the described symptoms above, and in many ways it doesn’t. I don’t really get pain near the knee. It starts at hip level on the outside of the left buttock and goes down the outside of the leg about half way. When it’s really bad, I might feel it as far down as the knee. I’ve been doing the clamshell, and bridges and other exercises for almost 4 months to get rid of it. While I haven’t completely stopped running or riding a bike, I’ve curtailled my activity alot. Does this sound like an IT Band issue or could it be something else? I’d appreciate any feedback.
Hi Dave. Hard to diagnose without actually being able to see you. Since you’ve had the pain for a while, I would invest in a trip to the orthopedist or a good sports PT. Sometimes, just getting an accurate diagnosis can help target and focus the rehab process.
Dave,
Did you ever get a diagnosis of your injury, just your symptoms are very similar to mine.
Dave your issues sound identical to mine. Pain starts at the hip and then works its way down towards the knee. The hip pain sets in anywhere between 7-14km on my run. I am doing hip strengthening, stretching, core strengthening and just can’t seem to get rid of the ITB pain. And i am doing my first marathon in 2 months time. I’ve found what helps the most is to adjust my gait and posture (as in Chi running).. If there was a magic pill to cure IT band pain, I’d love to know!
Thanks for sharing Nicole, if we discover that magic pill, we will let you know, but until then, just keep listening to your body, and keep up the posture changes if that works for you!
I just wanted to say thank you very much for this helpful and well-researched article. There is so much conflicting advice online but this all makes sense. I will be doing those strengthening exercises from now on! I might still be able to run my marathon in April now after all! 🙂
Thanks, Cate! Good luck and hope your marathon training goes great!
I was looking for the six-week gluteus medius strengthening program you wrote about in your article. Thanks
I’ve been struggling off an on with IT band pain for a couple of years now. I’ve read all about it and I know that hip exercises are supposed to be the way to get over it, but I find that whenever I do the exercises or stretches, it just makes my IT band pain flare up again. It seems like it makes things worse rather than better! I’m planning a big vacation in a couple of months that includes backpacking, so I’d love to get this IT band stuff behind me once and for all. Any advice?
Hmm, that’s a tough situation. My advice would be to tackle the pain first. Meaning, don’t start the exercises until you are feeling 100%. Then, once you have the pain managed, start with the exercises and continue with the therapy as if the leg was injured. After a few weeks, you should be able to do the exercises pain-free and then be able to run/walk
I have had IT band issues for about 4 months now, I have been doing the strengthening exercise for 2 weeks, managing up to 3 sets of 30 on everything but the lying hip abduction (which hopefully wont be too far off). IT band feels looser and definatly more comfortable, but im really concerned as when i feel down the outside of the leg (vastus lateralis) there are what feel like large knots and lumps? Ive tried massage and foam rolling but wont break up, any ideas or advice would be great please.
Have you tried more advanced massage techniques like Graston or ART? These might be able to get those final knots out.
Great article and description of the exercises.
Kind of a segue from Dave’s question. I have had tension (and only very slight pain) on the outside of my right hip for almost 4 years. It also cracks sometimes, while the other side does not.
I took up running again 6 months ago, but needed to stop when I developed sharp pain on the outside of my right knee.
I only connected to the two to IT band upon reading these types of articles.
In addition to the stereotypical symptom of sharp pain in the knee, I have the tension and weak pain in my hip, and do you believe this accompanying (and possibly less common?) hip tension differentiates me from what is typically recommended for runners with IT problems as described in this article? Thank you!
Sorry, second question here. I read the article from the Stanford group. I wonder, do athletes ever over-strengthen their injured side? That is, do they ever follow this sort of protocol only to reverse the strength/flexibility imbalance and develop IT-band injury on the other side? Thanks :o)
Hi Stella,
First, I don’t think your hip tension/weakness in the knee is any different than the norm. Your pain/symptoms just happen to manifest itself at the actual point of origin.
As for “over strengthening”, I don’t think this can happen (although I’ve never studied it). Theoretically, you could over-rely on one leg, but if both hips are strong it wouldn’t hurt. Plus, it’s always a good idea to balance by doing some of the same exercises on both legs.
i have struggled with many injuries over the past twenty years itb the most common. i ran new york half after a patch of never running better in my life and itb showed its face at 4 km. i ran through it, took three weeks off completely and ran Paris Marathon. both knees went at 8km….. stupidly hobbled through. after 6 weeks of strength rehab i am having a bilateral itb release in an hour…. will keep you all posted. remember this is a last resort after twenty years of running and many marathons xxx
Just wondering if anyone has had cortisone shots in legs or hips?
My legs are just getting worse, it has been a year now, no running, no cardio, standing, sitting causes the pain down both legs burning pain
I have done physio, months of the runnersconnect it band protocol and any hip strength improvements can not be sustained. I have tried ART and dry needling results were poor
Depressed now, lost all the gains in fitness, put on 20 pounds and the pain and edema is brutal
Sports med doctors hvae not been helpful at Umich in ann arbor, cortisone shots are my last resort
This is a very good article, I started strengthening exercises but I feel spasms after Im lying in bed. Is it normal foor the first days?
I don’t have pain on the side of my knee unless something touches it then the pain is severe for a little while. Could this be the It band? Had this for a very long time.
I bought the runners connect program 8 months ago and I think it is awesome, I wish I bought it before I began running. Unfortunately my itbs has lasted 18 months and I have given up running for the foreseeable future. Surgery might be needed
I am so glad I found this website…. I am current doing the exercises for an IT/periformis injury I’ve had for a while…. I actually tore one of my glutinous muscles by being too vigorous with PT exercises. Since your website suggests exercises/ stretches it would be great to have a verbal explanation on how to do the exercises correctly along with the pictures .
Thanks, Cintra. We do have videos and more in-depth instructions. You can them here: https://runnersconnect.net/strength-training-for-runners/
It’s actually a great and useful piece of info.
I am satisfied that you shared this helpful info with us.
Please stay us up to date like this. Thanks for sharing.
Strggling with ITB for 2 months now – overuse injury. Have a marathon in 45 days. The intensity of pain has gone down but it surfaces in the first 2 kms only. I can manage upto 13 ton15kms – question is shall i continje to rest or shall i continue with some runs
It is going to be very difficult to complete your marathon as of right now if you are only able to manage up to 15k. These articles may help you a little to see if the pain can be lessened, but it is not likely to get any better, and 45 days is still a long time away. https://runnersconnect.net/running-injury-prevention/it-band-injury-runners-stretches-exercies-treatments/ and https://runnersconnect.net/running-injury-prevention/cross-over-gait-to-treat-it-band-syndrome/ Your body is going to need some time for the inflammation to go down. Have you tried active release therapy? Hope this helps, let us know if we can help any more!
Kudos on the article! Hip strengthening really WORKS.
I used foam rollers on my IT Band but it made the pain WAY worse. So many sources online said it would help, so I couldn’t believe it when I ended up using the rollers and found that it did the opposite of what they claimed. It seems like the word is spreading about the rollers though, as I keep finding more articles that advise against them. For example: http://www.kingbrand.com/Iliotibial_Band_Syndrome.php?REF=17PV159.312
If you’re considering using rollers, proceed with caution.
Hi Bob, thanks for sharing. That is often the case with foam rolling IT bands as we mentioned in the articles. Wish you could have found ours first. Hope your IT band continues to improve now you are avoiding the foam roller with it!
Thanks for a great article. I’m exactly a week out from my first half marathon and did my ‘last long run’ before the event this morning and am no doubt suffering from this ITB pain in my left knee. Wanted to do 16kms but had to stop at 14km and then limped the rest of the way home. I’ve had similar pain in my left knee throughout my whole 6 months of training leading up to now but never even close to this extent and always resolves within hours after I finish my run. The pain can start at any time; sometimes in the first km and then sometimes like today, around 12km or so or any time in between. I’m feeling so gutted now knowing I might not be able give the half marathon a go let alone even finish it. Sad knowing I’m otherwise fit enough to do it other than my knee after all this training. Any tips or advise for me given my story? I’m icing and using NSAIDS….. 🙁
Hi Hannah, thanks for reaching out. Sorry to hear about your pain, but may we warn you that both icing and NSAIDs are not a great idea for your IT band! Here is why https://runnersconnect.net/running-injury-prevention/ice-running-injuries/ and https://runnersconnect.net/running-injury-prevention/are-anti-inflammatories-the-right-choice-for-treating-injuries/. This post may also be helpful as you may be making some of these also https://runnersconnect.net/running-training-articles/recovery-mistakes/
As for your race this weekend, you would probably be best to give yourself a few days off right now, and then run in the days leading up to the race. This is not the time you want to run through the pain. I am sorry to hear about it, and I know rest is the last thing you want to do, but the adrenaline may help you get through the race (then you will need to rest), but if you really want to get to the start line, taking a few days would be your best bet. Follow the other suggestions we mentioned in this post, and that will give you your best chance. If you do not get to race, all your training is still in there, and you will be able to build upon that in your next half marathon training 🙂 Stay positive! Hope this helps!
Hi there,
I’ve been struggling with ITBS for 6 months now. I stopped training almost immediately and have done nothing but stretching and strengthening of the glutes and hip flexors at home. Also in that time I have seen 5 different people (a collection of PTs and masseurs) and spent enough money for a two week vacation. They have all agreed on a diagnosis but everything they have tried has failed so far. I am, arguably, no better than I was 6 months ago. I tried to go out for a run last week and was in pain after 5 minutes. It took 3 days for the pain to subside.
Is it possible to have permanent ITBS? Have you ever come across a case where all the right things have been done but it has never made any difference?
I’m at my wits end to be honest.
Hi Neil, sorry to hear about your pain. Have you tried using the exercises we suggested in this post. I know it is not what you want to be doing as you have tried everything, but we have found runners have a lot of success healing their ITBS through this guide we have here. Unfortunately, it is not going to go away until it its treated correctly, and your PTs and masseurs have not found the correct solution so far. I know this is frustrating, but we hope you will give our guide a try. Hopefully this helps!
Fаbulouѕ, what a website it is! Thіs web site gives usefuⅼ іnformation to us, keep it up.
I have a new case is ITBS and I love your website. I am trying to do the hip strengthening exercises and I struggle with the Standing hip abductor and Hip hikes. When I put the weight on my injured knee I have weakness and I can’t do the exercise. Is this common or have I been misdiagnosed?
AWESOME BLOG , GREAT INFORMATION.