As much as we love having you check out our page, and we want to get to know you better, you are probably not here because you want to be.
If you are reading this article on knee pain, you are probably suffering from some runner’s knee symptoms, and are looking for something….anything to help it get better so you can get back to running.
Are we talking to you?
You are in the right place.
We will help you; determine if you do have this frustrating injury; what causes it, tips for preventing runner’s knee in the future; and many treatments ranging from conservative techniques like stretches to aggressive exercises for runners knee (even if you do not want to go to physical therapy).
This guide should give you some peace of mind, so your body can get back to healing, rather than dealing with the stress of the unknown.
Let’s get you back to running shall we?

What is a Runner’s Knee Injury?
Patellofemoral pain syndrome, sometimes also called “runner’s knee,” is the most common of all running ailments, accounting for 16.5% of injuries according to one recent study.
It’s characterized by a dull pain that is “behind” or “around” the top of the kneecap.
Typical aggravating movements include squatting, running (especially downhill), descending stairs, and prolonged sitting.
This makes training particularly difficult, and can mean you are forced to throw your plans out the window.
If you have patellofemoral pain syndrome (PFPS), you will also likely have pain when resisting leg extension, and possibly tenderness if you push against the kneecap itself.
Now:
It is important to distinguish PFPS from patellar tendonitis, which is an entirely different injury with a different treatment—patellar tendonitis manifests as pain into the tendon that connects the kneecap to your shin, the patellar tendon.
Patellofemoral pain syndrome is more common among women, though the reasons are not entirely clear.
The oft-cited “Q-angle” theory, which claims that women are more prone to knee injuries because they have wider hips, has been shown to be false.
Additional commonly-cited theories like leg length discrepancies and pronation are similarly unhelpful.
Patellofemoral pain syndrome gets its name from the relevant anatomy around the knee: the cause of the pain is the kneecap—the patella—rubbing against the groove in the femur, where it slides back and forth when you flex and extend the knee.
What are the Causes of Runner’s Knee?
Historically, research on PFPS focused on factors that affected the motion of the kneecap, particularly how the quadriceps control how the patella “tracks” in the femoral groove.
Indeed, scientific research has showed that people with poor quadriceps and calf flexibility, poor vertical jumping ability (which is highly dependent on your quads), and weak quadriceps are all risk factors for PFPS.
Blame was often ascribed to a small muscle on the outside of your thigh, called the VMO, which seems to fire differently in people with PFPS. And runners who did exercises that were designed to target the VMO often recovered!
Interestingly:
Recent research has demonstrated that these gains were probably from improvement in general quad strength, not VMO activation. And unfortunately, many runners don’t find relief from doing only quad strength, more exercises are needed.
What is the Treatment for Runner’s Knee?
Fortunately, research in the last ten years has uncovered another mechanism that contributes to knee injuries in runners: hip mechanics.
It turns out that, while it appears that the kneecap “tracks” towards the outside of your leg during squatting and running motions, it’s actually the femur rotating underneath the kneecap.
Check this out:
This explains why many runners (particularly women) with patellofemoral pain syndrome have weak hip abductors and external rotators. This seems to contribute to altered biomechanics when they run. Because of their muscular weaknesses, their knee “collapses” towards the center of their body when they run.
Some work has focused on directly altering the biomechanics of runners with patellofemoral pain syndrome by using a treadmill and camera system to provide gait analysis in real-time.
Unfortunately, this is not an option that’s widely available to most runners. Fortunately, some preliminary research has shown very good results from hip strengthening exercises and techniques. Specifically, the literature demonstrates that a successful program should definitely incorporate hip abductor, external rotator, and quadriceps strength.
Many programs that have produced good results also include hip flexor/extensor strength, closed-chain “functional” exercises like squats, and balance training.
RunnersConnect Bonus
Download our Top 5 Runner’s Knee Prevention Exercises for Free.
It’s a PDF with the 5 best exercises to help you prevent runner’s knee.
How Else Can I Limit the Time Off Running From Runner’s Knee?
For most runners, a dedicated strength training program will be what ultimately provides relief from patellofemoral pain.
But as usual, there are other treatments that can either provide temporary relief or act as a supplement to your strength training.
Stretching and foam rolling can be a great adjunct to strength training and can loosen up tight calves and quads.
Often, running on an injury will leave you with tight and stiff muscles, which a foam roller and some quad stretching can loosen up. Just take care not to stretch if it irritates your knee.
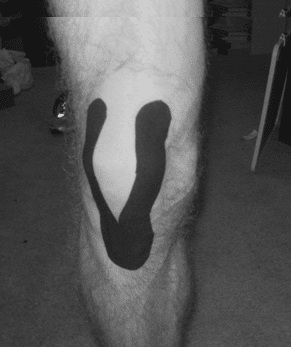 Applying tape, using either rigid athletic tape in a patellar taping, or with a flexible kinesiology tape, has been shown to provide some relief to athletes with patellofemoral pain.
Applying tape, using either rigid athletic tape in a patellar taping, or with a flexible kinesiology tape, has been shown to provide some relief to athletes with patellofemoral pain.
Some research has also indicated that knee braces (cho-pat straps, neoprene sleeves, and similar devices) may also provide some relief.
This is crazy:
It seems that the mere presence of the tape or the brace, which provides some tactile feedback on the skin, provides most or all of the relief, not so much the way in which it is applied or the mechanics of how it affects the knee. So a loose “improper” taping helps just as much as a tight, correct taping!
Another option is a product called NuNee. NuNee is an innovative new product designed specifically for Runner’s Knee. NuNee was invented by 2x Ironman Mike Emmerling because of his own 5-year struggle with Runner’s Knee. The research reveals that if you relieve the pressure you relieve the pain. NuNee does exactly that. By relieving the pressure on your patella (knee cap) NuNee can provide immediate relief of Runner’s Knee pain.
You might be wondering:
Custom orthotics may speed the pace of your recovery, but at least according to one study, they don’t appear to exert much of an influence after several weeks of rehab. This obscures the fact that many runners have found significant relief from custom orthotics (though others have not), so you may consider them if first-line treatments are not working for you.
But given that there is little or no evidence that factors below the knee (i.e. the feet and ankles) play a role in the development of PFPS, custom or even over-the-counter orthotics should not be your first choice in treating patellofemoral pain syndrome.
Outline of Conservative Treatment:
1. Hip and quadriceps strength exercises:
- Abductors—lying side leg lift or band abduction
- External rotators—lying “clam” or band external rotation
- Quadriceps—straight leg lift
A good starting place is 15 of each, once per day. As your strength improves, you can move to two or even three sets of 15 each. All exercises must be done SLOWLY!
2. General lower leg strengthening and balance
- Balance, possibly on unstable surface (foam pad, bosu ball)—start with 30sec or 1min, build as much as you like
- Mini-squats on a step, starting around 15 repeats and working to two or three sets
- Glute bridge—start with 10-12 10-second holds, build toward 2min continuous
3. Icing after each run
4. Quadriceps and calf stretching.
5. Quadriceps and calf foam rolling
6. Patellar taping, either with traditional athletic tape or flexible kinesiology tape
Aggressive Treatment:
These options are often more expensive or difficult to obtain and should be reserved for cases of PFPS that don’t improve despite several weeks of strength work, rest, and other rehab.
1. Gait analysis at a physical therapy office equipped with a treadmill and a high speed camera to detect and correct gait abnormalities
2. Custom orthotics may alter your gait and relieve stress on your knee, but it is also possible that they may not help at all.
When Can I Return to Running?
Patellofemoral pain is notorious for sticking around for weeks or even months, so do be cautious with this injury. In general, you don’t want to run through pain.
Sometimes, as you are recovering, your knee may feel a bit stiff at the beginning of a run, but as long as it gets better, not worse, as you progress in your run, you are probably okay to keep going.
What’s the bottom line?
It’s difficult or impossible to predict how much time off you’ll need, especially considering the biomechanical roots of this injury.
Most treatment plans that are published in scientific journals consist of 4-6 weeks of exercise and no aggravating activities (including running), but all cases of an injury are different.
Remember:
You actually will not lose as much fitness as you think in those first few weeks, so it is better to let it heal.
You may only need a few days off if you catch it early, but if you’ve been running on PFPS for a while, you may need a lot longer. A good doctor or physical therapist can often give you a decent estimate of how long it will take you to return to running.
In the meantime, you should stick to cross-training activities that don’t hurt your knee.
Aqua-jogging, biking, and using the elliptical are all options, but you’ll have to see how these affect your knee. If a cross training activity hurts your knee, you shouldn’t be doing it!







17 Responses
I love this! This is an awesome article, it really answered a lot of my questions as far as what to do and how too! Thanks. I’ve been trying to do a lot of research on runners knee because it’s something I have been dealing. I will share this information and I would also like to post a link to this other awesome article I found about runners knee, incase someone comes across this and want to find out more just like me. 🙂
http://teamdoctorsblog.com/2012/05/25/cracking-achy-knee-pain-or-chondromalacia-patella-treatment-and-prevention-tips-from-the-barefoot-running-doctor/
I’m a victim of runner’s knee, worst injury ever!! I like your tips & advice for recovery. In my experience the epsom salt bath worked sometimes, but sometimes it triggered pain too. Mine was really wacky, kept me off running for 4 months. I can’t stand runner’s knee. I hate that every time I run it’s always in the back of my mind that it can flare up again. I’m sorry to hear it lasted so long. It’s the worst! http://www.mykneestretches.com/
Thanks so much for this article. It’s the best one I’ve read yet! I was first diagnosed with ITBS then PFPS. I still am getting pain on the outside and below the kneecap area around 3-4 miles. Feels like my knee just locks up and needs “popped” out. I’ve run many marathons, so I know pain, but this is not something I can run through. I am curious if you have a checklist to determine which injury I actually have!? Very frustrated and becoming depressed! SOOOO want to run long distance again. Help!
I can attest to the importance of stretching the hams and glutes. I had noticed a lot of tightness and have really been focused on my stretching. It has really made a difference. Thanks for confirming that I have been doing the right stretches. I look forward to trying the strengthening tips!
This has helped me a lot! I have experienced so much lower back and gluteal pain. I literally get knotted up so tight. The lateral band walks hit the spots! Thank you!
Good insight into the importance of whole body mechanics and the hip joint in the etiology of runner’s knee. I send many patients to physical therapists with experience in treating this condition as you describe – focus on the core / hip as well as the knee / foot. Thanks.
I’m trying not to self diagnose but I’m sure this is my problem too! Great article! Does anyone have pain while they are In Bed at night also? Mine seems to seize up, I try to keep it straight to reduce the pain as this is more comfortable? Even walking up the stairs hurts too? Any feedback appreciated as started training again this week after having a baby and my knee is in agony already
My son suffered from very accute runners knee as a result of over pronated ankles (i.e. flat feet). Kept him out of sports and PE. We did all the exercises, every night for years. He was in custom orthotics and seeing all sorts of Drs. Then, about 2 years ago, NIH published a paper on slant-board squats. Magic! They worked. He just ran a 5k in highschool pain free. Look it up and do them very slowly on the way down.
Hi Steve, thanks for sharing your sons findings, we go over exercises like those in our prevention routine that readers can download to return to running as quickly as possible, we also recommended the slow part too! Glad to hear your son is healthy again, make sure he keeps them up even after his pain goes away, it will help prevent future issues!
I am wondering when should I go to the doctor? I haven’t been running this week since the pain started. It is getting a bit better. I work at a school and so have had to go up and down stairs quite a bit so that might make it harder to heal. Right now my insurance isn’t great. In a month, I’m getting married and going on my fiance’s insurance, which is a lot better and then I won’t have to worry. But if it would go away with stretches/exercise/rest, that would be nice. I don’t want it to turn into a serious issue, obviously, however. Thank you!
Hi Kristen, thanks for reaching out. Sorry to hear about your knee pain. It would be best to check in with the doctor as soon as possible if you are able to. If it is going to be too expensive, give the suggestions in this guide a try to see if they help alleviate your pain. It is good you are being proactive about it. Continue to be smart with your training, and listen to your body. Hopefully by now it is feeling even better!
I’ve been running only for a year now but was loving it so much decided to book a half marathon for this October, I had booked this way in advance to get my fitness up and started my long distance 2-3 months ago, I was so wary of injury so made sure I slowly increased my long run and eventually got to 10 miles and stuck to this for 4 weeks until I got used it, I then fell over while running and banged both knees, since then I tried going out for a run and my right knee starts hurting within 1 mile and by 2 I have to stop. When I walk straight after it becomes worse and when climbing stairs etc, I had a few weeks off and tried a small run this morning which ended badly as it came back straight away! I’m so gutted because the half is only 3 weeks away and absolutely devastated that this has happened so close! I really don’t know what to do I’ve trained so hard now I worry I have to pull out. 🙁 any suggestions would very much appreciate!!!
Hi Lucia, unfortunately it would be impossible for us to tell you what exactly is going on with your knee. Your best bet would be to go to a doctor to find out what is going on and ask their advice. If you can cross train, we would definitely recommend this during this time to maintain fitness, and then you will still be strong enough to do the half marathon, but if you are unable to do this, then it might be best to back out of the marathon. If you are truly loving running, then you will persevere during this time, and that is one of the best things about running….there are always more races coming! Yes, you may have to back out this one, but look at how far you have come, and you should be proud and happy that you have found something you truly love! If we can help with anything else, let me know 🙂
Some great info. I had runner’s knee after running my first marathon. It’s frustrating because you want to run but you know you have to rest. i tried lots of different methods to treat it and found acupuncture to be very helpful as well as strengthening the hips and knee itself.
Hello,
I went to doctor about pain around left knee. I was given xray and told to go to physical therapy. When i completed physical therapy i continued doing exercises to build strength. Pain around right knee imoroved a lot but have pretty bad chronic pain around left knee. I quit doing the exercises and kniw have to start doing again. I think this all started because i was doing a lot of standing (have flat feet and had gained a bunch of weight). It hurts so much when I sit a lot like at movies etc. and I am very upset, discouraged by it when it flares. I put ice, take aspirin, put on absorbine junior etc. (I am trying orthopedic arch supports of all kinds for my poor flat feet) and helps some for while. I hope and pray pain goes away and I never need surgery. I have endured other bad chronic pain for other problem. It gets discouraging. I seriously do not want or need this kind of pain. I am seriously thinking of not working anymore because I stand for hours and often around my knee and feet bad. Can you please offer me any other good advice? I know my It band often gets tight and I sometimes use roller on or massage IT band but cannot understand why it gets so very very sore. I read that bicycle riding will build cartilege (but you should have saddle high enough so knees are not bent too much as this could cause more pain). Thanks for your help. Good luck to all.
New here – recreational runner 5k, etc., trying to know why knees have become weak, and both appear to have a thick band horizontally across immediately below kneecaps – help! Thank you.
this good site for get simple with biomechanical explanation to remember at treatment time thanks runner connect team by fahis
physiotherapist