You cross the marathon finish line feeling strong, wave at the crowd, and eat your celebratory bagel.
Two days later, you wake up with a sore throat and a fever.
Your first instinct is to blame the race.
Your second is to worry you did something wrong with your training.
Your third is to figure out why this happens to so many runners.
Post-race sickness is real.
It’s not a sign of weakness or poor fitness.
It’s a predictable immune response to extreme exercise, and your body’s reaction to a marathon is documented and measurable.
So, in this article you’re going to learn the research-backed practical advice on: runner’s flu and how to prevent it.
- What runner’s flu actually is and why the “open window” is real physiology
- How common post-race sickness is among marathoners
- Why your immune system crashes after intense exercise
- When you’re most vulnerable and how long that window lasts
- Which factors increase your infection risk the most
- Evidence-based prevention strategies that actually work
- How to recover faster if you do get sick
What Is Runner’s Flu and Why Does It Happen?
Runner’s flu is not actual influenza.
It’s a temporary vulnerability to upper respiratory tract infections (URTI) that appears in the days following intense endurance exercise, particularly marathons.
This vulnerability exists because your immune system temporarily suppresses its defenses after extreme effort.
The window of suppression typically lasts 24 to 72 hours post-race.
Research has shown that runners have significantly higher risk of upper respiratory tract infection within 1-2 weeks following marathon completion.
This phenomenon is called the “open window” theory of exercise immunology.
The term describes a specific period when your body is more susceptible to pathogenic invasion because your immune cells are recovering and your mucosal barriers are temporarily weakened.
The open window is not a myth or a nocebo effect.
It’s measurable immunology backed by decades of peer-reviewed research on exercise physiology.
Post-race sickness is a predictable side effect of pushing your body to its limits, not a failure of your immune system.
How Common Is Post-Race Sickness Among Runners?
Between 30 and 60 percent of marathon participants experience upper respiratory tract infection symptoms within 1-2 weeks of race completion.
This high prevalence appears consistently across studies of recreational and competitive marathoners.
Your chances of getting sick are closer to 1 in 3 rather than 1 in 10 or 1 in 5.
Psychological stress and sleep loss amplify this baseline risk.
Runners who sleep poorly in the week before the race or who report high pre-race anxiety have significantly higher infection rates than those who sleep well and manage stress.
Age also matters.
Older runners (55+) show lower infection rates than younger ones, likely because their pre-race training stress is lower.
If you got sick after a marathon, you’re statistically in the majority, not an outlier.
Why Does Your Immune System Drop After a Marathon?
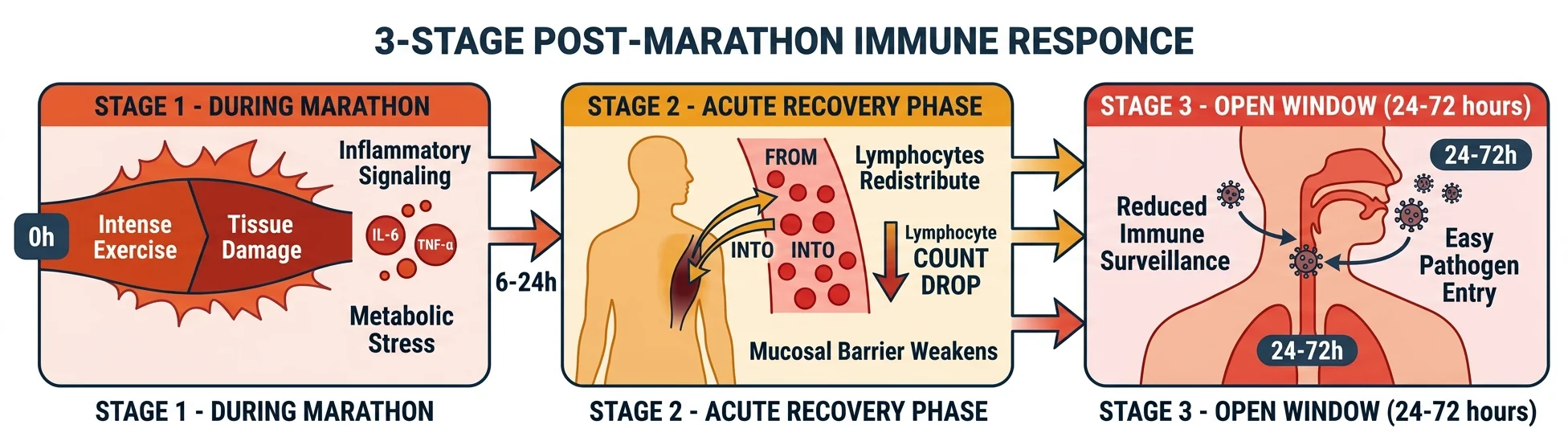
During a marathon, your body produces massive amounts of inflammatory signaling molecules called cytokines, particularly interleukin-6 (IL-6) and tumor necrosis factor-alpha (TNF-α).
These cytokines trigger an acute inflammatory response that mobilizes immune cells to manage the tissue damage and metabolic stress of the race.
In the hours immediately after the race, your circulating immune cells (particularly lymphocytes) drop sharply as they redistribute from the bloodstream into damaged muscle tissue and other affected areas.
This redistribution creates the vulnerability.
Your upper respiratory tract loses circulating immune surveillance precisely when pathogens have the best chance of invading, because the mucosal barrier also weakens temporarily.
The mechanism is not broken immunity.
It’s recovery-phase immunosuppression.
Your immune system is not weak.
It’s redirecting resources toward tissue repair and adaptation.
That redirection leaves a temporary gap in your defenses against incoming pathogens.
Research demonstrates that anxiety and stress hormones amplify this post-exercise immunosuppression, making the window wider and more vulnerable for runners with high pre-race anxiety.
This is why managing stress before a marathon is protective.
Lower pre-race cortisol means less inflammatory cascade post-race, which means faster immune recovery and a shorter vulnerability window.
Your immune system response to exercise is measurable and reproducible across thousands of athletes.
This is textbook immunology, not an individual weakness.
The sicker you get post-race, the better your endurance fitness, because only maximum-effort races trigger the profound immune redistribution that creates vulnerability.
How Long Does Your Immune System Stay Suppressed After a Race?
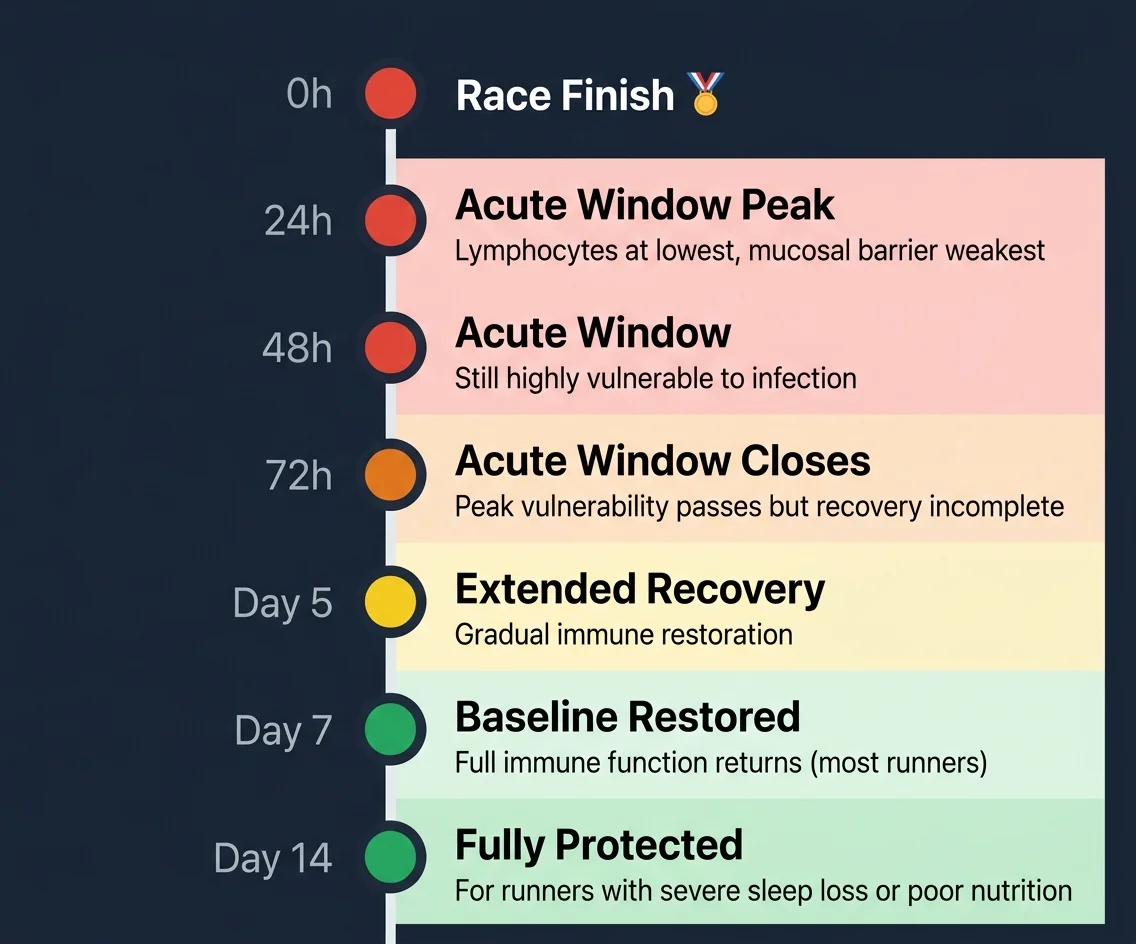
The acute open window is the period of greatest vulnerability, lasting between 24 and 72 hours post-race.
This is when your lymphocyte counts are lowest.
Your mucosal IgA (the antibody protecting your upper respiratory tract) is most depleted.
Pathogenic invaders have the easiest entry point during this window.
However, your immune system doesn’t snap back to baseline after 72 hours.
Recovery is gradual, with full restoration of pre-race immune function taking 5 to 7 days for most runners.
If you experienced severe sleep loss or poor nutrition during race week and recovery, restoration can take up to 2 weeks.
This extended timeline explains why many runners get sick days after the race rather than the day after.
They encounter a virus on day 3 or 4 but think they’ve cleared the danger zone.
Then they develop symptoms on day 5 or 6 when they’re already training again.
The 72-hour window is the peak, but your immune vulnerability extends across your entire first week of recovery.
What Factors Increase Your Risk of Post-Race Sickness?
The open window exists for every marathoner, but not all vulnerabilities are equal.
Several factors determine whether you get sick or stay healthy during that critical recovery period.
Sleep deprivation before the race. Runners who average less than 6 hours per night in the week before a marathon have 3-4 times higher infection rates than those sleeping 7-9 hours nightly.
Sleep loss amplifies the inflammatory cascade post-race and slows immune cell recovery.
A single good night’s sleep before the race can’t undo a week of poor sleep, but prioritizing sleep 2-3 weeks before race day measurably protects your immune system.
High pre-race anxiety. Psychological stress elevates cortisol, which directly suppresses immune cell function and prolongs the inflammatory response post-race.
Runners who report high anxiety in the week before a marathon show wider and more severe open windows.
Poor post-race nutrition. Your immune cells repair and multiply using amino acids and glucose.
If you don’t eat within 1-2 hours after finishing, you miss the critical window for refueling the immune recovery process.
Continued hard training immediately post-race. Runners who don’t take 3-5 days of easy effort or complete rest after a marathon extend their immunosuppression.
Additional training stress prevents immune cell recovery.
Crowd exposure and hygiene. Marathons mean race expos, finish lines, and celebration gatherings all with high-pathogen-density environments.
Touching your face during these 24-72 hours post-race dramatically increases infection risk.
Dehydration and electrolyte depletion. Severe dehydration impairs immune cell function and delays recovery of mucosal barriers.
This is why post-race hydration and electrolyte replacement matter as much as carbohydrate and protein.
Sleep, nutrition, stress management, and recovery days matter more than genetics in determining whether you get sick post-race.
How to Prevent Post-Race Sickness: Evidence-Based Strategies
You can’t eliminate the open window because it’s a necessary part of the recovery process after extreme effort.
But you can shrink it, and you can manage your behavior during those vulnerable days to dramatically reduce infection risk.
Sleep 7-9 hours nightly starting 2-3 weeks before the race. This is the single most protective intervention against post-race sickness.
Consistent sleep quality builds immune reserves that persist through race week and accelerate post-race immune recovery.
Manage pre-race anxiety through evidence-backed practices. Meditation, structured breathing (4-7-8 breathing), journaling, or coaching conversations with your training partner reduce cortisol elevation in the days before the race.
These practices measurably shorten your post-race vulnerability window.
Eat a post-race recovery meal within 1-2 hours of finishing. Carbohydrates plus protein plus electrolytes in that window replenish glycogen stores.
They provide the amino acids your immune system needs for cell repair and multiplication.
Recovery nutrition targets: 40-60 grams of carbohydrates, 15-25 grams of protein, and 300-500mg sodium within 60 minutes of finishing.
This doesn’t need to be a formal supplement.
Real food (sandwich, chocolate milk, pasta with sauce) works just as well.
Take 3-5 days of easy or complete recovery after the race. Your marathon recovery plan should include zero hard efforts for the first 3-5 days.
This gives your immune cells time to recover without the additional metabolic stress of training.
Limit crowd exposure for the first 48-72 hours post-race. Skip the post-race party.
Avoid touching high-contact surfaces and your face.
Hand hygiene matters more during this window than at any other time in your training.
Hydrate aggressively for 24-48 hours post-race. Rehydrate to 150% of the body weight lost during the race over the 4-6 hours post-finish.
This accelerates immune recovery and restores mucosal barrier function.
The strongest predictor of staying healthy post-race is whether you take true recovery days, not whether you buy specific supplements.
Can Supplements or Vitamins Prevent Runner’s Flu?
Runners often ask whether vitamin C, zinc, probiotics, or other supplements can prevent post-race sickness.
The research is mixed, which means the practical recommendation is clear: focus on fundamentals first.
Vitamin C. The belief that megadoses of vitamin C prevent colds dates back to a 1970 claim that has never been replicated.
A Cochrane review of 29 trials found no benefit from supplemental vitamin C for reducing cold incidence in the general population, including physically active individuals.
Zinc. Some evidence suggests that supplemental zinc (15-30mg daily) taken during heavy training blocks and in the week before a race may modestly reduce infection duration if you do get sick.
Prevention is unclear.
Probiotics. Probiotics are popular but evidence is limited.
A few studies show specific strains may modestly reduce infection rates in runners, but the effect is small.
Most probiotic supplements lack the specific strains used in those studies.
Immunoglobulins and IgA-boosting supplements. These are emerging interventions with interesting mechanistic rationale because they directly address mucosal barrier function.
Current studies are small, but early data suggest potential for specialized formulations in future research.
Save your money on supplements and focus on sleep, nutrition, stress management, and recovery days first.
How to Recover Faster If You Do Get Sick
Despite your best prevention efforts, you might still get sick.
If you do, several strategies can shorten illness duration and reduce severity.
Rest completely for the first 3-5 days of symptoms. Training while sick extends inflammation and delays immune recovery.
The sickness is telling you that your immune system is working hard.
Help it by removing additional stress.
Eat adequate protein and carbohydrates.
Your immune system needs raw materials to fight infection.
Aim for 1.2-1.6g protein per kilogram of body weight daily during illness.
Maintain carbohydrate intake to support immune cell energy demands and prevent additional metabolic stress.
Sleep as much as possible. Sleep is when immune cells proliferate and cytokine balance restores.
Prioritize 9-10 hours nightly if you’re sick.
Rehydrate and replenish electrolytes. Fever and congestion increase fluid loss.
Drink water consistently, not just when thirsty.
Include electrolytes (sodium, potassium) because immune cell function depends on proper electrolyte balance.
Return to training conservatively. Resume running only when symptoms resolve.
Start with easy 20-30 minute efforts.
Wait at least 1 week before resuming any hard efforts or long runs.
Watch for warning signs. If fever persists beyond 5-7 days, if you develop chest pain or shortness of breath, or if symptoms worsen after initially improving, contact a doctor.
Most cases are viral and resolve on their own, but bacterial infection or viral complications warrant medical attention.
Sick runners who rest recover faster than those who train through illness.
Runner’s flu is post-race upper respiratory infection caused by temporary immune suppression after marathon effort, known as the “open window.”
Between 30 and 60 percent of marathon runners experience illness within 1-2 weeks of racing, with vulnerability highest in the first 72 hours and gradually recovering over 5-7 days.
Your immune system doesn’t fail after a marathon. It redirects resources from infection defense to tissue repair, leaving your upper respiratory tract temporarily vulnerable to pathogens.
Sleep deprivation before the race, high pre-race anxiety, poor post-race nutrition, and skipped recovery days are the primary modifiable risk factors.
Prevention focuses on sleep (7-9 hours nightly 2-3 weeks pre-race), pre-race stress management, post-race nutrition (within 1-2 hours), 3-5 recovery days, and limiting crowd exposure during the first 72 hours.
If you get sick, rest completely, eat adequate protein and carbohydrates, sleep 9-10 hours nightly, stay hydrated with electrolytes, and delay return to training until symptoms resolve.
Supplements like vitamin C show no benefit, and zinc and probiotics have limited evidence.
Focus on sleep, nutrition, stress, and recovery before considering supplements.
The most predictive factor in staying healthy after a marathon is whether you actually take recovery days, not your genetics or training volume.





