Sharp pain along the inner side of your ankle that worsens with every mile.
A dull ache that climbs your shin after a few miles.
Tenderness when you press directly on the tendon just below the bony bump on the inside of your ankle.
If any of that sounds familiar, you may have posterior tibial tendon dysfunction, one of the most underestimated running injuries.
Unlike most soft tissue injuries, this one can permanently change the shape of your foot if you keep running through it.
The good news: catch it early, follow the right protocol, and full recovery is possible without surgery.
In this guide:
- How to self-test for posterior tibial tendon dysfunction in 60 seconds
- Why the injury worsens when you run through it, and what the 4 clinical stages mean for your treatment
- How long the healing timeline actually takes (10 to 16 weeks for most runners)
- The 4-step conservative protocol backed by clinical research
- What cross-training preserves your fitness while you recover
What Is the Posterior Tibial Tendon?
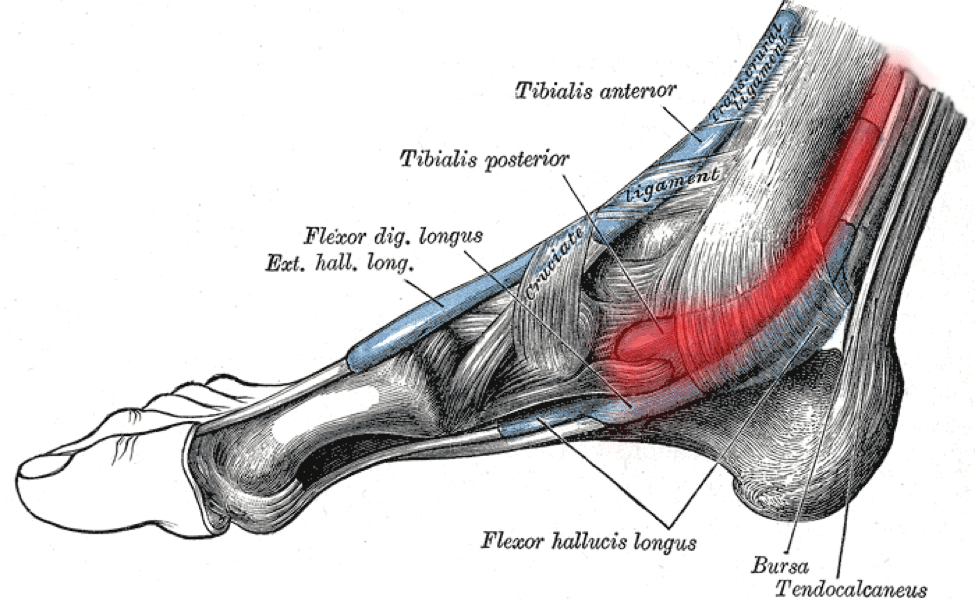
The posterior tibial tendon runs along the inside of your ankle, connecting the tibialis posterior muscle deep in your calf to the bones of your foot’s arch.
The tendon itself is no thicker than a pencil.
But its job is enormous.
Every time your foot hits the ground and pushes off, the posterior tibial tendon locks your ankle in place and holds your arch rigid under load.
Without it, your arch collapses inward, your ankle rolls, and everything upstream has to compensate.
In advanced posterior tibial tendon dysfunction, that arch collapse becomes permanent.
Think of your foot’s arch as a suspension bridge, and the posterior tibial tendon as the main cable holding tension.
Weaken that cable and the bridge sags.
What Are the Symptoms of Posterior Tibial Tendonitis?
The hallmark symptom is pain along the inner ankle and foot, sometimes extending a few inches up your shin.
There may be mild swelling, and the area will be sore to press directly on the tendon.
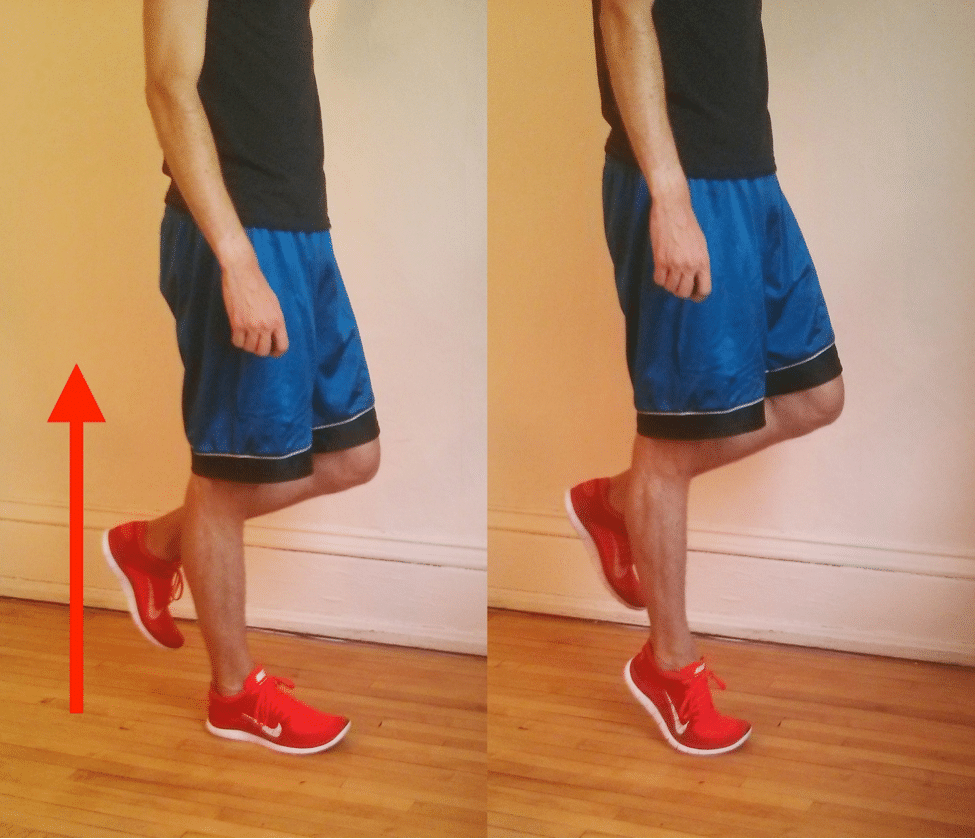
The most reliable way to identify this injury yourself is the single-leg heel raise test.
Stand on the affected leg with your knee straight.
Rise up onto the ball of your foot as high as you can, hold for a second, then lower slowly.
Pain or weakness along the inside of your ankle during that movement is the clearest at-home indicator of posterior tibial tendon dysfunction.
In more severe cases, you won’t be able to rise onto your forefoot at all.
Research has used the single-leg heel raise as an inclusion criterion in posterior tibial tendon dysfunction studies, reflecting how specifically it identifies the injury.
This test also helps rule out injuries with similar locations.
Medial tibial stress syndrome and stress fractures of the medial malleolus produce pain in the same region but don’t cause ankle weakness on the heel raise.
RunnersConnect Bonus
Download our Posterior Tibial Injury Outline for free.
It’s a PDF with the conservative and aggressive treatment options for runners suffering from Posterior tibial tendon pain
Can You Run With Posterior Tibial Tendonitis?
Running on a posterior tibial tendon that’s already damaged is what turns a manageable injury into a permanent one.
Here’s why.
Research has shown that the posterior tibial tendon has a zone of relative avascularity in the section wrapping around your medial malleolus.
Poor blood supply means slow healing.
Running adds new damage faster than a poorly-supplied tendon can repair it.
As the tendon weakens, your arch drops and your foot pronates more under load, which puts more stress on the tendon, which causes more damage.
That cycle compounds until, in severe cases, the arch collapses permanently.
The 4 Clinical Stages
Doctors classify posterior tibial tendon dysfunction in 4 progressive stages.
Your stage determines your treatment options.
Stage I: Tendon inflammation or microdamage, but no change in foot shape. Conservative treatment works well. This is where you want to catch it.
Stage II: The tendon begins to elongate and the arch gradually flattens. Most patients at this stage can no longer complete a single-leg heel raise. Conservative treatment is still possible but requires more intensive management, often with specialized ankle-foot orthoses.
Stages III and IV: Partial or complete tendon rupture with permanent foot deformity. Surgery is usually required.
The 4-step protocol below applies to Stage I. If you’re in Stage II or beyond, see a podiatrist or foot and ankle orthopedist before starting any rehab.
What Causes Posterior Tibial Tendonitis in Runners?
The most common cause is classic overuse: ramping mileage too fast or resuming training too quickly after time off.
Acute tears from a fall or sudden ankle roll are less common but do occur.
Runners with high arches carry some protection since the tendon doesn’t have to work as hard to maintain arch position.
Runners of every arch type still develop this injury.
A case-control analysis of 2,002 running injuries found posterior tibial tendon dysfunction to be relatively uncommon at rank 26, but among the most consequential when it does occur.
How Long Does Posterior Tibial Tendonitis Take to Heal?
Stage I cases treated consistently with the full protocol take 10 to 16 weeks from the start of rehab to return to running.
The two most comprehensive clinical studies on conservative treatment ran 10 to 12 weeks (Kulig et al., 2009) and 16 weeks (Alvarez et al., 2006), including an initial 2-week rest period.
Walking does not need to stop, but it should be minimized during the early weeks, especially on uneven surfaces.
Wear supportive shoes during all waking hours, including around the house, to reduce tendon load on every step.
The 10 to 16 week window assumes no setbacks.
Runners who continue any activity that loads the tendon during that period extend the timeline significantly.
Every clinical study that has successfully treated posterior tibial tendon dysfunction with conservative measures included arch support as a component of the protocol from day one.
The 4-Step Treatment Protocol for Runners
The research on conservative treatment points consistently to 4 components working together.
No single piece works in isolation.
Step 1 — Stop Running and Reduce Load
Stop running completely.
The posterior tibial tendon heals slowly because of poor blood supply to the section wrapping around your medial malleolus.
Running adds damage to a structure that can’t repair itself fast enough to keep pace.
Swimming and cycling are generally safe as long as they’re pain-free.
Aqua jogging is the best option for maintaining running fitness during this phase (more on that below).
Keep daily walking to a minimum, especially on uneven surfaces, and always in supportive shoes.
Step 2 — Support Your Arch With Footwear and Orthotics
Arch support reduces the mechanical demand on a tendon that can’t currently handle full load.
When your arch is propped up, the posterior tibial tendon doesn’t have to work as hard with every step.
One study in the conservative treatment literature asked patients to wear shoes and orthotics for at least 90% of waking hours, including barefoot time at home.
Walking barefoot on hard floors still stresses the tendon.
Wear your shoes from the moment you get up.
On custom versus over-the-counter: the comparison hasn’t been studied specifically for posterior tibial tendon dysfunction.
What the research does establish is that some arch support is clearly better than none.
Whether you need custom orthotics is a question for your podiatrist.

Step 3 — Stretch Your Calves Twice Daily
3 separate clinical studies that successfully treated posterior tibial tendon dysfunction each included a structured calf-stretching protocol.
The standard protocol:
- 3 sets of 30-second wall calf stretches with a straight knee (targets the gastrocnemius)
- 3 sets of 30-second stretches with a bent knee (targets the soleus)
- Done twice daily, on both legs
- Use an incline board if you have one
One important detail from the Kulig et al. 2009 USC study: do all your stretching in your shoes and orthotics.
The support changes the mechanics of the stretch in a way that’s relevant to how the tendon loads.
Step 4 — Progressive Tendon Strengthening
This is where the research gets specific, and where most informal rehab advice falls short.
The protocol has 2 phases.
Don’t move to Phase 2 until you’ve completed at least 3 weeks of Phase 1.
All exercises are done in shoes and orthotics. Stop if you feel significant pain.
Phase 1: Build Endurance (Weeks 1-3)
- Seated sole-to-sole: Sit with feet on the floor. Press the inside edges of your feet together and hold briefly, then release. Start with 4 sets of 25 reps daily, building over 2 weeks to 12 sets of 25, then to 300 continuous reps.
- Theraband dorsiflexion (200 reps, 1x/day): Loop a theraband around the top of your foot and anchor it in front. Pull your toes toward your shin against resistance. Progress to a stronger band when 200 reps feels easy.
- Theraband inversion, endurance (200 reps, 1x/day): Anchor the band at 45 degrees. Roll your foot inward against resistance. Keep a towel under your foot. All movement from the ankle only.
- Theraband eversion (200 reps, 1x/day): Same setup as inversion, but roll the foot outward.
- Theraband inversion, strength (3 sets of 15, 2x/day): Same inversion movement with the heaviest theraband you can control for 15 reps. Slow and controlled in both directions. Increase resistance as the tendon adapts.
Phase 2: Functional Loading (Week 4+)
- Single-leg heel raises: Stand on the affected leg, rise onto your forefoot, lower slowly. Start with a few reps and build progressively to 50 continuous reps. Use a wall lightly for balance only.
- Toe walking: Walk forward on your toes with heels fully off the ground. Start at 8-10 yards and build to 100 yards (91 meters).
- Balance board tapping: Stand on your affected leg on a balance board. Tap the board in each of 5 directions (forward, back, left diagonal, right diagonal, rotational), 20 taps per direction. Repeat in reverse for 2 full sets.
Plan on 3 months of daily work across both phases before attempting a return to running.
What Cross-Training Can You Do While You Recover?
Aqua jogging is the best option for this injury.
It closely mimics running mechanics with zero imp






18 Responses
I struggled with PTT for years, and it ultimately ended my collegiate career. I finally overcame it years later with a combination of orthotics, clamshell strengthening, topical anti inflammatories, and support shoes. But the key was finding a good self massage technique. Slowly rotating the foot while working my thumbs up the tendon and muscle behind the ankle bone and up the shin finally got everything to relax.
Thanks for sharing Stuart!
I enjoyed reading this article and i have developed this injury (that i have never had before,even from running on the treadmill,too fast for too long)..I cycle much more than running,because i was cycling between 16 and 32 miles everyday for work and.I changed my job to a local job and i wasn’t doing all the cycling mileage everyday and two weeks ago i used my turbo trainer on my bike and cycled at 22 mph for 20 mins doing this three times,so 1 hour cycling at 22 mph. That was enough to give me this injury for the first time .I have learnt more valuable lessons from doing too much exercise,too fast for too long!!!.Also look how quickly my fitness from cycling 16 to 32 miles everyday to only cycling 4 miles to work everyday dropped my fitness like a stone and that is why i have got this injury when i cycled for 1 hour at 22mph after six weeks of only cycling 4 miles a day.I am just going to rest,rest and more rest until this injury has gone and then have to build up my cycling fitness again.I can lift my left heel with a little soreness,so i guess i’m still ok to make a full recovery with rest over time,i hope so.Thanks Bruce
Mine is a longitudinal tear of the peroneal brevis tendon–the stabilizing tendon on the outside of the foot. Would these healing protocols work for me also? Thank you.
Hi Derrick, yes, many of the exercises we recommend throughout our posts are helpful for a variety of different injuries as they are strengthening all the muscles around the lower leg to prevent future injuries of all kinds. You may also want to check this one to out to make sure it is not weakness in your hip that is causing this injury https://runnersconnect.net/running-injury-prevention/the-relationship-between-hip-strength-and-running-injuries-the-latest-research/ Hope this helps!
Hi Coach Tina , I have PTT and a doc I went to see is recommending EPAT therapy. I don’t know of anyone that has done this so I am trying to get a perspective on this treatment to see if it worthwhile or not. I know it is relatively new ,but I dont want to waste $300.00 per treatment (3 are recommended) if it is just a scam treatment or hasn’t produced results for anyone else. Any advice you or anyone can offer me on this treatment ?
Thank you for this information on how to treat post. tib issues. For 8 months, I have been aching from what my new podiatrist thinks is an inflamed post. tib tendon being impinged by a talus that is rotated 40 or so degrees medically plus a torn, chronically sprained deep deltoid ligaments. I have tried two rounds of physical therapy totaling about 4 months, several injections including PRP and steroids, and significant reductions in my activity. It took me a few months to stop running entirely (I am obsessed running!). Finally I am non-weight-baring on my injured foot (just started week three of that). Do you have any conjectures on whether complete rest will finally help reduce my pain? I am also open to any additional advice you are willing to provide on how to treat this nagging injury. Finally, my advice for anyone with this injury is to stop running immediately.
Hi Katie. I realize it’s been a while since you posted. But I’m reaching out to you because I have the same problems. Are you available to chat on our similar conditions.? Mark
I, too, have been suffering from PTT for over 8 months. It has completely stopped my running. I kept thinking it was getting better so I would try to run again only to have it flare up but even worse. Now I am unable to run at all. I just completed 6 weeks of total rest, wearing an Aircast and using crutches. It did start to feel a little better but the swelling remains and the soreness is returning now that I am weight bearing again. Not sure what options that I have now other than surgery. I have found that few therapists understand this injury and more often than not they make the problem worse. I have been using topical anti inflammatory gel (Voltaren) but not sure it has made any difference. If anyone has any ideas let me know! This is a very frustrating injury and there is no quick fix, at least for me.
Hello, I am also suffering from this problem and my doctor advise is surgery. however the process seems worse then the problem it self.
i believe before going to these extreme one should try self healing. it is base on faith and the ability the body have to heal it self though faith in God.
As a follow up to my own post, it has now been 13 months dealing with this injury and it’s finally getting better. I am not running but I can now do all other activities with very little pain. I recently visited a great doctor at the Mayo Clinic. He is a sports orthopedic doctor. He talked to me about the Alfredson Protocol. Developed for Achilles injuries, it can be applied to this tendon. It focuses on strengthening the tendon while elongating it versus contraction exercises. It works. Google this. Respond if you’d like any more information. Good luck!
Hi, I don’t see a description of the “sole to sole” exercise. What is this?
Help! For 10 years I have had PTT issues. Dr. says that I no longer have a tendon-that it must have snapped. Who knows why. Not overweight and don’t really exercise or anything that would have strained it. I still have a high arch-always have. I wear orthotics and a brace. Sometimes I question the whole thing. This article talks about the foot becoming pronated and the arch falling. I have neither issue. I can’t stand on one foot on that foot and the foot is somewhat inward facing at the ankle. Going to go to a new doctor soon. This doctor made an Arizona brace for me, but come on! Who is going to wear that thing? It doesn’t even fit in a gym shoe and I have a professional job where I couldn’t wear gym shoes. Anyone ever hear of a PTT just snapping? Dr. says MRI shows that the tendon is missing. Anyone have any insight into a disappearing PTT? My issues seem different than the ones in the article and the comments.
Thank you for this informative post that finally revealed what I’ve been experiencing all these years. I’m not sure if I was born with this, but as a kid I would sometimes stretch after waking, and my foot would suddenly ‘lock’ with a sharp and intense pain. Only by pressing and rubbing the arch of my foot was I able to relax it. And I had no idea it’s related to the reason why my feet hurts after standing for long periods in the recent years. I’m gonna try those stretching exercises.
I may have early stage of this injury. My question is how do I know if it is posterior tibial tendonitis or the flexor hallucis longus? Are the treatments the same? When it first started I researched it a bit, started icing, and put my “good feet” arch supports in my work shoes. I plan on beginning this rehab regimen. Last thing I want is a flat arch!
Help please. i have ptti. my orthotic specialist has put a wedge in the medial forefoot region . Should it be placed in posterior(hindfoot,by calcaneus or forefoot?-
Dr Barry Shapiro
bps1@rogers.com
Chris said:
I’m in my 80’s, and although I’m not a runner I have been very active outdoors throughout my life. However, after a series of incidents since childhood, I now realize that earlier diagnoses as Plantar Fasciitis were hasty and incorrect, and that what I really have is Posterior Tibial Tendonitis! Now, I’m very pleased to have this information and the treatments provided on your website. For many years I’ve practiced a modified form of Trigger Point Therapy, and the patterns of pink and redness induced during my very brief treatment sessions match some of the illustrations shown on your pages. Thank you!
Feel free to delete this comment, but a chunk of this article above is repeated, which makes for tricky reading until you realize you can keep scrolling to get to the rest. It would be good to fix.