You feel it when you walk, you definitely feel it when you bend forward, and the idea of running faster than a shuffle sounds almost impossible.
Hamstring pain is a bad injury for anyone to deal with, especially for runners who need those hamstring muscles to be working correctly to do what we love the most.
The hamstrings are an essential muscle group in running.
They flex your knee and assist in hip extension, meaning they are active at multiple points in your gait cycle.
It does not matter if it is a sharp pain, aching soreness, pulling, tightness or even radiating up to your back, pain in the top of your leg where your hamstring attaches can make life a misery. If hamstring tendonitis is
We will do anything to make it better, even if it means spending thousands of dollars on controversial treatment.
While the most common hamstring injuries are acute or chronic muscle strains, they are also vulnerable to tendonitis at their origin, an injury termed high hamstring tendinopathy or proximal hamstring tendonitis.
While rare, this injury is difficult to treat and can become a prolonged and chronic problem.
The relatively limited scientific and medical reports extant are fairly recent, and as such, there are no solid numbers on what percentage of runners come down with it.
Today, we would like to give you the ultimate guide to these injuries. Explaining what hamstring tendonitis is, how you can test to see if you have it, many different treatment options ranging from conservative to aggressive, and how you can return to running as soon as possible.
If this is not enough, there is a great discussion at the bottom of the page, where you may be able to find additional information on what has worked for others suffering with the same condition.
Ready to find out what is really going on? Let’s do it.
What is Hamstring Tendinopathy?
The hamstrings run from the top of your tibia, just behind your knee, up along the back side of your thigh and towards your pelvis.
While one branch of the hamstrings attaches to the femur, the rest course up your thigh and underneath your glute muscles, attaching to the pelvis at a bony prominence called the ischial tuberosity.
These twin “peaks” of bone are sometimes referred to as your “sitting bones,” as they support much of your weight while sitting, especially on hard surfaces.
The junction between the tendons of the hamstrings and the ischial tuberosity is the area affected by high hamstring tendinopathy.
True high hamstring tendinopathy feels like a vague, aching soreness high up on your hamstrings and deep in your buttock.
There will be pain when you run, especially when accelerating and when maintaining a fast pace.
Sometimes the sciatic nerve, which passes very close to the ischial tuberosity, can become irritated as well, resulting in pain that radiates down the back of your thigh.
In addition to pain while running, you may feel irritation at the ischial tuberosity while sitting on hard surfaces. It also may hurt to press directly on the ischial tuberosity.
How Do I Know If I Have Hamstring Tendonitis?
A review study published in January of 2012 outlined three physical tests for high hamstring tendinopathy.1
The first is a simple standing hamstring stretch, where you rest your foot on a knee- to waist-high support and stretch your hamstrings.

The second is an assisted hamstring stretch, done while you are lying on your back. With your hip and knee flexed, an assistant slowly straightens your knee to stretch the hamstring.
It may be possible to replicate this test without an assistant by using a rope or a belt, as pictured below.
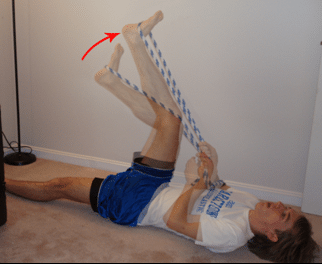
The third test is similar to the second, but this time, the knee is rapidly straightened by an assistant. High hamstring or buttock pain with any of these three tests is indicative of high hamstring tendinopathy.
While these tests were fairly accurate, correctly identifying between 76 and 89 percent of the injured runners, none were perfect, highlighting the usefulness of high-tech imaging to accurately diagnose or rule out high hamstring tendinopathy.
MRIs can be very fruitful in evaluating hamstring injuries, as described by Marc Sherry of the University of Wisconsin in a recent review article.2
An MRI can spot tendon thickening, tearing, inflammation, and swelling in the bone at the ischial tuberosity. Ultrasound can also used, but unlike an MRI, it can’t visualize bone marrow edema.
What if I am not sure if this is hamstring tendinopathy after all?
If the three tests above did not seem to match your pain, it may not be proximal hamstring tendonitis.
A host of other injuries can cause deep buttock pain, including piriformis syndrome, muscle strains, a sacral stress fracture, or pain radiating from low back injuries, so you may want to go read more about those.
How do I Treat My Hamstring Pain?
In one of the few comprehensive articles on treatment for high hamstring tendinopathy, Michael Frederickson, William Moore, Marc Guillet, and Christopher Beaulieu at Stanford University provide a very insightful outline of treatments their group has found helpful for high hamstring injuries in runners.3
After the diagnosis has been confirmed with a physical examination and MRI scan, the injured patient is evaluated for core strength, hamstring flexibility, and pelvic stability.
What will help to speed healing?
Frederickson et al. recommend that any pelvic tilt be corrected (presumably by manual or chiropractic manipulation, though the article does not specify how), as it can increase hamstring tension.
They also endorse soft-tissue work (like massage) to break down scar tissue along the proximal hamstring tendon, though the authors caution that direct compression of the ischial tuberosity should be avoided.
Other case studies have also supported the usefulness of soft tissue manipulation, including techniques like ART and Graston, for the treatment of high hamstring tendinopathy.3
Gentle stretching of both hamstrings several times a day is also encouraged. We would also encourage you to include as many of these recovery foods into your diet as possible to help your body fight back.
How do I strengthen my hamstrings?
But as Frederickson et al. point out, the core of their rehabilitation program is eccentric strengthening of the hamstrings.
Like the patellar and Achilles tendons, the tendon at the origin of the hamstrings is thick, fibrous, and has a poor blood supply, which makes healing difficult.
Additionally, much like in these two more common tendon injuries, tendonitis of the high hamstrings appears to be a degenerative process, not an inflammatory one.4
This means that the fibers of the tendon are becoming frayed, damaged, and disordered.
However, because we know that both Achilles tendonitis and patellar tendonitis can be effectively treated with eccentric strength exercises, it is quite logical to base a rehab program for high hamstring tendinopathy around eccentric exercise as well.
The strength rehabilitation program begins with simple isometric hamstring and glute exercises like glute bridges.
As soon as these are tolerated, Frederickson et al. recommend progressing towards eccentric exercises as soon as the introductory exercises can be done without pain.
A standing “hamstring catch” exercise can serve as a good introductory eccentric exercise, and Frederickson et al. endorse Swiss ball curls as ideal for development of both eccentric and concentric strength.
These Swiss ball curls can be progressed as tolerated, moving from short range of motion to full range of motion and eventually, single-legged Swiss ball curls.
RunnersConnect Insider Bonus
Download our full High Hamstring Recovery and Prevention Routine inside your Insider Members area.
It’s a PDF with images and descriptions of the most effective prevention and rehab exercises for runners with High Hamstring issues.
Frederickson et al. also emphasize the importance of core strength in hamstring injury rehabilitation, citing another study which found that core strengthening reduced the risk of recurrent hamstring strains.
It’s possible that a strong abdomen and hip musculature can stabilize the pelvis, taking strain off the hamstring.
Frederickson’s paper focuses on the use of plank exercises, particularly with leg lifts incorporated to encourage coactivation of the glute and hamstring muscles, as a key component of recovery.
I am Desparate! Is There Anything Else I Can do to Speed Healing of My Hamstring?
Other options discussed in the Fredericson et al. paper include corticosteroid injections and extracorporeal shockwave therapy.
Both of these treatments have the potential to weaken the tendon, so they are reserved as ancillary treatments, not a sole basis for recovery.
Steroid injection
Corticosteroid injections are better understood, and while injections directly into the tendon itself can be quite harmful, Fredericson et al. write that, by using ultrasound imaging to guide the injection needle, the anti-inflammatory drug can be delivered to the irritated tissue surrounding the tendon without penetrating or damaging the tendon itself.
They also found that patients whose MRIs exhibited more swelling around the ischial tuberosity and less thickening of the tendon got more relief from a cortisone injection than patients with more pronounced tendon thickening.
Extracorporeal shockwave therapy
Shockwave therapy is mentioned briefly, as it has been found to be effective in other types of chronic tendon injuries in athletes,5 though Fredericson et al. caution that they have little experience using it for high hamstring tendonopathy and that animal studies have shown that it results in a drop in tendon strength (at least in the short term).
Surgery
In a small number of cases, surgery is necessary to relieve tension on the sciatic nerve and divide up the fibrous and damaged tendon near the ischial tuberosity.
The good news is that, according to a 2009 study by Lasse Lempainen and coworkers in Finland, a high percentage of athletes eventually return to the same level of sport after being referred for high hamstring tendinopathy surgery.6
Eighty of the 90 patients referred in Lempainen’s study made a return to the same level of sport, with 62 of them having “excellent” results.
While this is encouraging, the mean recovery time of five months (and ranging from two to twelve) is sobering and serves as a reminder that few surgeries for a running injury are ever really “minor” when it comes to time off from running.
Why is hamstring tendonitis so difficult to get rid of?
High hamstring tendinopathy is a persistent and difficult running injury to overcome.
Additionally, due to its relative rarity (especially outside of running) and the paucity of good review studies on potential treatments, the evidence for solid treatment protocols is still lacking.
On the bright side, however, since it’s known to be a degenerative tendon issue, the same treatment strategies that work with injuries to the Achilles and patellar tendons should also be effective with high hamstring tendinopathy.
As Frederickson’s article outlines, a progressive strength program to strengthen the core, improve glute strength, and promote healing in the proximal hamstring tendon through eccentric exercises should be at the heart of any rehabilitation program.
Due to the similarity of some of this injury’s symptoms with other hip injuries, it’s important to get a proper diagnosis; this will likely entail a physical examination and an MRI.
Additionally, because of the individual nature of this injury, it’s recommended that you find a good orthopedist and physical therapist to supervise your rehabilitation and advise you on your return to running.
Who should I talk to?
If you have been dealing with this for an extended period of time, and still find no relief, these are some experts to consider talking to.
Talk to your physical therapist
See a physical therapist or chiropractor for manual therapy, massage, ART, or Graston Technique to break down scar tissue and adhesions in the high hamstring area.
Make sure the practitioner focuses on the muscle and tendon tissue and avoids the ischial tuberosity—you don’t need any additional irritation there. many runners also find sitting on a tennis ball or other hard surface when traveling or sitting for long periods of time to be helpful when first standing up.
Talk to an orthopedist
Your orthopedist may be able to say whether a corticosteroid injection is right for you, preferably guided by diagnostic ultrasound imaging.
According to Fredericson et al., this can be especially helpful in cases where an MRI shows significant swelling near the ischial tuberosity.
Talk to a doctor
Consider talking with your doctor about the risks and benefits of extracorporeal shockwave therapy.
While it’s unproven in high hamstring tendinopathy, it has shown some success with chronic tendon issues elsewhere in the body.
Cross Training While Injured and During Recovery
Cross training is recommended while you're injured and as you slowly return to running.
The best form of cross training for this injury is Aqua Jogging. Studies have shown that aqua jogging can enable a well-trained runner to maintain running fitness for up to 4-6 weeks.
Aqua jogging is a form of deep water running that closely mimics the actual running movement. Your feet don’t actually touch the bottom of the pool, so it is zero impact and safe for almost any type of injury. In my experience, the only time to avoid aqua jogging is when you have a hip flexor injury, which can be aggravated by the increased resistance of the water as you bring your leg up. Because aqua jogging closely mimics natural running form, it provides a neuromuscular workout that, in addition to aerobic benefits, helps keep the running specific muscles active. The same can’t be said for biking and swimming. The only downside to aqua jogging is that you need a pool that is deep enough to run in without touching the bottom. If you’re lucky enough to have access to a pool of this size, aqua jogging should be your first cross training choice.In one study, a group of ten runners trained exclusively with deep water running for four weeks and compared 5km race times pre deep water running and post deep water running.
The researchers found no statistical difference in 5k time or other markers for performance, such as submaximal oxygen consumption or lactate threshold.
In a second study, researchers measured the effects of aqua jogging over a six week period.
This time, 16 runners were separated into two groups – one who did aqua jogging workouts and the other who did over land running.
Using the same training intensities and durations, the researchers found no difference between the groups in maximal blood glucose, blood lactate, and body composition.
It get’s better:
Research has also demonstrated that aqua jogging can be used as a recovery tool to facilitate the repair of damaged muscles after hard workouts.
These findings make aqua jogging an important recovery tool in addition to being the best cross training method for injuries.
Need one more reason?
The calories burned aqua jogging are even higher than running on land, so if you want to avoid weight gain while you take time off from running, this is definitely the exercise for you!
Aqua Jogging Workouts For Runners
If you're interested in aqua jogging to rehab your injury, then the absolute best way is to use one of my favorite programs, Fluid Running.
First, it comes with an aqua jogging belt and waterpoof bluetooth headphones so you have everything you need to aqua jog effectively.
Second, they have an app that pairs with the headphones so you can get workouts, guided instructions on how to aqua jog properly, and motivation while you're actually pool running.
This has been an absolute game changer for me when I am injured.
I used to dread aqua jogging workouts because they were so boring and it took all my mental energy to stay consistent.
But, with workouts directly in my ear, it's changed the whole experience and I actually look forward to the workouts. So much so that I now use aqua jogging as a cross training activity in the summer, even when I am not injured.
Fluid running is an awesome deal when you consider it comes with the belt (highly recommended for better form), the waterproof headphones (game changer for making pool workouts fun), a tether (to add variety to the workouts you can do) and the guided workout app (to make your cross training structure and a whole lot more interesting).
That's why we've partnered with them to give you 2 additional running-specific workouts you can load into the app when you use the code RTTT .
Check out the product here and then on the checkout page, add the code RTTT in the coupon field and the workouts will be added to your order for free.
If you'd rather do the aqua jogging workouts on your own, here are some great ideas to get you started!
Medium Effort Workouts
The Pyramid
10 minutes easy warm up - 1:00 hard, 30 seconds easy - 1:30 hard, 30 seconds easy - 2:00 hard, 30 seconds easy - 2:30 hard, 30 seconds easy, go to 5:00 in 30 second intervals and then come back down the pyramid (4:30 hard, 30 easy, 4:00 hard, 30 easy etc). Finish with 10 minutes easy cool down.
Wave your hands in the air like you just don’t care
10 minutes easy warm up, 1 minute medium (87-92% of maximum heart rate or what feels like tempo effort), 1 minute sprint (95-100% of maximum heart rate or all out sprint), 30 seconds hands in air (keep moving your legs in the running motion, but put your hand above your head), 1 minute rest, Repeat 10-15 times. 10 minutes easy cool down.
Hard Workouts
One of the difficulties of cross training is replicating those truly lung-busting, difficult workouts.
So, if you’re going to be pool running quite a bit due to injury or limited training volume, invest in a bungee cord designed for sprinters.
Tie one end of the resistance band to a sturdy object (pole, lifeguard stand, pool ladder) and bring the other into the water with you.
Put the strap around your waist and begin aqua jog away from your starting point.
You’ll begin to notice the bungee tighten and resist against you (depending on the length of your pool, you may need to wrap the bungee around the supporting object or tie it in knots to make it shorter to feel resistance).
Spend a few moments testing yourself to see how far you can pull the bungee.
This is a great challenge and a fun way to compete with yourself during an otherwise boring cross training activity.
Now for the hard part:
Pick a point on the pool wall or side of the pool that you feel stretches the bungee to a very hard sprint that you could maintain for 60-90 seconds.
This will be your “sprint” marker that you’ll use on sprint intervals (95-100% of maximum heart rate or all out sprint).
Now:
Find a point that feels like the end of a hard tempo run.
Mark this spot as your “medium” interval distance.
When you complete the hard workouts, you can use these reference points to ensure that you maintain a very hard effort.
The springboard
10 minutes easy warm up, 90 seconds easy (slowly moving out and stretching the bungee), 2 minute medium, 1 minute sprint, 1 min rest (let the bungee pull you back – this is kind of fun). Repeat 10 times. 10 minutes easy cool down.
The race simulation
10 minutes easy warm up, 90 seconds easy (slowly moving out and stretching the bungee), 5 minutes medium (focus and concentrate, just like during the hard part of a race), 30 seconds sprint, 2 minutes rest. Repeat 4 times. 10 minutes easy col down
The lactic acid
10 minutes easy warm up, 90 seconds easy (slowly moving out and stretching the bungee), 2 minutes sprint, 90 seconds rest. Repeat 12 times, 10 minutes easy cool down.
I guarantee that with the bungee, you’ll get your heart rate through the roof.
You can challenge yourself and make aqua jogging more fun by seeing how long you can stay at your maximum stretched distance or seeing how far you can push it.
Likewise, if you have a friend who is injured (or someone willing to be a good sport) you can try pulling each other across the pool for some competitive fun.
Cross training can be tough, especially when you’re injured or want to be increasing your volume faster.
However, I hope that providing a variety of workouts, either through the Fluid Running app (which also makes it easier to keep track of the workout while in the water) or on your own can add a fun challenge in the pool and you can emerge from your injury with minimal fitness loss.
How Can I Get Back to Running?
High hamstring tendinopathy is reported to take a long time to recover from.
Of the few case studies on runners with high hamstring tendinopathy, all report recovery times on the order of 8-12 weeks,8 a timescale echoed by Fredericson et al.
Cross training activities should not stress the lower legs until the bent-knee stretch test can be done without pain; at this point, activities like cycling and pool running can be incorporated into your routine.
Once you can perform a back plank with leg lifts pain-free on both sides (pictured below) and have normal range of motion, you can being the gradual return-to-running program outlined here:

| Week 1 | Walk 5min / jog 1min, build to 5 sets on alternating days(ex. 2x5min/1min, off, 3x5min/1min, off, etc.) |
| Week 2 | If no pain, walk 5min / jog 5min, build to 5 sets on alternating days |
| Week 3 | If no pain, advance to 20min jog, no more than 5 days per week |
| Week 4 | If no pain, advance to 20min run at normal training pace, no more than 5 days per week |
| Weeks 5-8 | If no pain, gradually increase running speed, volume, and acceleration as tolerated |







156 Responses
Great article Jeff. I wonder if any of my previous hamstring pain was de to this although never as irritated while running, mostly sitting. Ever since I have begun religious about core, isolated stretching, and foam rolling, there have been no flares ( knocking hard on wood). Thanks for all of your great advice
I have been suffering with this high hamstring pain in the butt pain.., I go to chiropractor and I started with deep tissue massage.., have not been to orthopedic yet but am about to call for an appnt. I discovered i cannot sit for lengthy times now with this pain..this all just started a few weeks ago..been treating it myself Chiropractor suggetsted stretching ; I am afraid to do this without a proper MRI…first (don’t want to injure a possible tear) I am not a runner but am a walker and hiker..love being outdoors..! I am sure the orthopedic Dr. will send me to PT…hoping it works…been sitting on icepacks also..never ever had ths injury and I used to ski alot back in the day…I am approaching 65 and hoping this pain will go away!!
Hi Lorraine, sorry to hear about your pain, hope the discussion in this article brought you some comfort that others have found relief through alternative methods. We also have an article we released today about eating as a master, hopefully this will help your body bounce back a little quicker! https://runnersconnect.net/masters-running/master-runners-change-eating/
I’m pretty sure this is what I’ve got along w/my pelvic stress fracture. I’m not sure if the fracture is the result of ignoring it for so long. I knew I had recurrent issues w/my hamstring and that I could not do a bridge or stretch effectively. Despite this I started training for a marathon and got up to 50 mile weeks before the thing went pop. What was most disturbing for me is there was no pain until it went. I had two separate weeks when that leg painlessly collapsed after speed work when we were doing our quick bursts but during my daily runs, no issues. Saw a PT, she told me to keep running so I planned another 2:30 long run. I actually did feel relatively good the first hour but then after that it went quickly downhill and I knew I was done. I hope I can get myself back into shape without this thing haunting me going forward.
I am assuming I have this. I experienced the exact symptoms yesterday. I have to sit all day (desk job) and this is really bothering my condition. I’m not a runner but a long time spinner. Thanks for the article and exercises to help improve it. This injury is literally a pain in the behind!
Wow, I’m so glad I found others with same problem. I injured myself at 9 mile mark in NYC Half marathon. Was on track for 7minute pace finished the last 4 miles at 11min per. Its 2 weeks and pain is still too great to run.
Sitting in my vehicle is the worst.
I really need to run, I run every day and have another half marathon first sunday in May.
have you been to a ROLFER?? ITS like a heavy duty massage that uses deep manipulation of the bodys soft tissue to really get in and work out that injury. i am going and it is working and feels so much better. it relieves chronic pain, and reduces stress.
google it and read about it…might be what you need.
get well and so you can run strong.
Sitting is the worst! I find the only way to survive sitting for long periods either driving my car of sitting at my desk is using a square thermalite camping pillow that one can purchase online or at any camping shop. they semi inflate and you can add more air if necessary. Also it is discreet and can be rolled up and taken anywhere, like the cinema or out for dinner.
Thanks for your input Jennifer! Many of us find sitting for long periods causes pain, just more evidence that we were not meant to sit so much! That is a great idea to use the camping pillow, I am sure our readers will find that very helpful! Thanks for the suggestion 🙂 Glad it has eased your pain!
Great article, Jeff. Thanks so much. The best thing I’ve read in my continual research of high-hamstring tendinopathy. Much appreciated!
I’ve had this off-and-on for five years, and had little success in getting rid of it, and it’s driving me crazy — and I’m thinking about surgery.
And yes, like Alan said, sitting in a car for long stretches is positively the worst, for some reason
I know this discussion is about two years old, but I am desperately looking for relief. I have been struggling with upper hamstring pain for almost 7 years on and off. It’s getting worse and my activity level and abilities have plummeted. I read what you shared and that you were considering surgery. Did you ever get it done? If so, did it help? I think it’s my only answer. It’s not even as much about returning to running as it is about being out of constant pain! Would really appreciate anything you have to share about this. Thanks!
Hi Cheryl, hopefully one of the other readers will fill you in on their thoughts. Sorry to hear you are in constant pain. Have you been following the treatment options we talked about in this article? Some of the other readers in this post have talked about some alternative treatments that helped them. You may want to consider trying some of them. Let us know if you need anything else from us!
I’m also really struggling on a daily basis with this pain and Physio has repeatedly failed me. Do you happen to know what surgery actually enatails for HHT and what the success rate is? Thanks
I’m 50 years of age and very active. I’m almost certain I have it…I did see a orthopedist and started PT in October 2014. I have stopped running 3 months ago and just stopped all lower body exercises, boot camps, spin etc. a few weeks ago. My cardio consists of swimming with pull boney and the elliptical. I continue to strengthen and have started a procedure called Dry Needling. It’s getting better but it’s a slow process…I feel I’m still 6-8 weeks away…UGH. To be smart I should confirm diagnosis with a MRI.
That would be a good idea Dan, then at least you can put your mind at rest! At least you have been able to keep up with some activity. Let us know how you get on.
Hi, I have just been discussing this with my sports injury specialist as I have suffered with it for about 3-4 years. Surgery was discussed as a final option but it is major and, according to him, has about a 50-60% success rate. It also has a 9+ month recovery time – so not something to be taken lightly at all.
You are definitely right! It is a serious decision to make, and one that runners need to make sure they have done their research for. Thanks for sharing your thoughts!
Well, almost a year on from my first post about this and I have had EST (electroshockwave therapy), continuous physio strengthening of hamstring and core, botox injections in piriformis muscle, steroid injections around the hamstring tendon, anti inflammatory medication, Pregabalin (nerve medication to try to reset pain signals) and guess what? NOTHING HAS CHANGED at all, whilst muscle strength is much better, if anything I am perhaps one or two points worse on the sensitivity/pain and bare in mind I have been standing to work daily for over 2 years now too.
So, getting close to agreeing surgery on the tendon to remove the thickening etc and perhaps see if the sciatic nerve is tethered to the tendon at all. Orthopaedic surgeon and neurosurgeon have both reviewed and seems the tendon is very likely the main cause (thickening etc).
Anyway – seems I have at least another 4-6 months of work (assuming surgery can happen in the next 2-3 weeks) to be able to sit/stand/run pain free.
For what its worth, I have remained running (gently) more or less throughout though if it is bad then the cross-trainer on a high resistance is totally pain free so at least I can burn some frustration out that way.
I have been struggling with this since last July. I’m a mountain biker and I didn’t understand the signs early on. I haven’t been on the bike since. While it has improved and I’m not in pain these days I know that a flare up can be caused by the slightest thing. I wanted to share that I’ve recently been working on the elliptical doing both speed and resistance and focussing on my heels to concentrate on building strength in my hamstring. It doesn’t aggravate it and seems to be helping. The recommendation to stretch scares the heck out of me. It seems the slightest stretch reignites the pain.
Hi Kelly, sorry to hear that, biking does not sound like fun with the hamstring pain. Thanks for sharing what works for you, that will give others something to think about if they are running out of options. Did you try the recommendations on here (other than the stretch?), they may help you continue to improve, just be very gentle….as you have learned!
My daughter, gymnast, had this and we got the MRI, showed swelling at ischial. She overstretched her split. You need to get this checked to see what you are dealing with–we were doing gentle stretching, but after going to PT she was told NO stretching–and is in a 3 phase PT program which should last about 6 weeks. She has had great results so far—the PT is not difficult, but she can do NO gymnastics–nothing that will tweak that area at all. Definitely frustrating, but worth the time off.
Thanks for sharing Monica, we hope it continues to improve for her!
Late reply, but I am very flexible (and 50 year old male) and always have been (flat hands on the floor, no knee bending at all). Since last Feb when I started to see the physio I was also told no stretching other than quads. Whilst it seemed strange at first, it is now completely normal (though as you will see from above the work did not help).
Did I hear five years, how depressing, Ashby do you keep on reinjuring it. Did you try total rest for an extended period of time
Thanks so much for the information- I got this injury a few weeks ago while cross-country skiing when one ski came to a sudden stop and I felt the tendons tear as I fell forward- immediate pain-
Have had issues with this for 7 months. Had 2 prp injections, and though it has improved, I am still not doing big miles or speed work. Have been trying to strengthen core and hammys. This looks like a great article and will certainly use some of the info. Have 5 months till Melbourne marathon, am hopeful of competing there. Was training for this event last year when injury occurred. Am running 6-7km runs now but not fast, trying to build. Still gets sore but hard to tell exactly what triggers pain, as some days it hurts and others it does not, even though training schedule is the same. It still hurts to sit longer than 5min. I am sure of one thing. It is a long term injury and you have to work hard at it. Good luck to all.
Man…I’m fairly sure this is what I have. Ended up snapping it during some sprints. Been about a year or so and it’s so annoying. Gonna get on this workouts and hopefully they’ll get me somewhere. Fantastic, article!
I’ve had this off and on for about 2 years, rest, stretch, gradually get better, gradually get back into working out – no long runs, then boom – the cycle starts again. Right now I’m in the I can’t sit because of the pain from my butt to my front shin phase.
Has anyone heard about ultrasound therapy? I’m just doing research and hear that by applying the ultrasound it actually encourages blood flow to help heal.
I’d welcome any advice on healing/relief, and how to overcome.
Thanks!
I’ve been diagnosed with this and been in rehab for this for 18 months. I’ve not run or biked at all since diagnosis in March 2012. It has not gotten better, only worse. It has made my life not even worth living since I can do no exercise any longer.
look up ROLFER. AND see if you this helps. its a holistic way of improving injuries and getting rid of them. its like a massage on steroids..haha but it does work
Well I’m convinced this is part of what afflicts me. Sitting is very painful and I carry a soft foam cushion everywhere with me. I’ve had this pain for over 6 years.
When it first happened I could hardly bear the pain as it radiated into my hip and my sciatic nerve often got extremely irritated. Still does every now and again. No doctor seemed to know what the matter was back then although they said the MRI showed inflammation at the ischail tuberosity. Tried a cortisone shot but it made no difference.
I was told to rest it and that it would improve after a few months. Well perhaps the pain got a little more bearable or I just have learnt to tolerate it. But I wouldn’t say it’s really improved. The hip pain is a lot less though.
Recently I have started had the hamstring (left leg) massaged. It feels like a tough old rope! Luckily he’s a wise massage therapist and did not touch the sit-bone. I’ll try these exercises out very gently and see what happens. The therapist thinks I also have weak glutes. I gave up running about 9 years ago from an ankle injury. I enjoyed running but no longer miss it.
I hadn’t realised that surgery was a possibility. I might consider that as a very last resort, but I’m a bit of a coward that way!
Have you had a chiropractor look at your lower back? I’ve had this problem for over 2 year now. I spend a lot of time and money with one sports therapist who just did lots of massage. I went to another and he said, ‘Scoliosis and trapped nerve’! He stuck his thumb into my spine and a couple of painful minutes later, it was, I reckon 70% better. The 30% remains (high tendinopathy) which is really stubborn but good to make some progress
I’m very happy and thankful to the author who published this. Although I am a dancer, not a runner, I felt the beginning symptoms of this while doing deep stretches and over splits in that exact area. Now I know what to do, this article saved me a lot of headache.
Very good article! Although the article states the injury as being rare, it seems a lot of runners get it. I never had a problem with running until now – in my 40’s. After a few years off, I started to gradually get back into running last year. 2 months went well but when I started pushing myself, my hips started hurting. I continued running through the pain until my right foot also started hurting. Then my knee and then my lower back and then my hamstrings high up were hurting. With 5 areas of pain, I went to a Chiropractor and he gave me a right foot heel lift. My knee pain was gone the next day. Eventually my foot got better. My hips got better and lastly, my lower back got better, For about a year, I still have high hamstring pain and just keep my strides short. I did this for months pushing myself further with low pain to no pain. I finally decided I needed to do sprints and fartleks if I was going to improve my time. That’s when my high hamstring flared up so bad I could barely walk. I’ve been sitting on a tennis ball at my desk job and also when I drive, stretching like crazy. I’ve started pilates and core strength training. I’m trying to refrain from running and just cycle until I can get back to running full stride. After a year of hamstring pain, I’m finally giving in to rest and recovery. Oh… I’ve found that biofreeze helps alleviate the pain so I’m now using that daily to help the recovery faster. I refuse to have any type of surgery… Every injury I’ve ever had with just rest and rehabilitation, I’ve been able to overcome the need for surgery.
I’m 14 and i’ve been struggling with this for about 13 weeks. As i’m so young and this is an over use injury i think my rehab time might be slightly quicker than others but im not too sure when to start running again. I have had dramatic improvement after doing the nordic curl and squats and now i can lift my knee up sharply with no pain. The annoying this is, after so much improvement, i still cant do a one legged glute bridge pain free and after a run (that seems pain free) it will start hurting again when lifting my knee. I’ve missed the whole track season and i hope to be back for cross country. This has been very useful.
This is a good article. I was doing taekwondo when i suddenly felt a pain in my high hamstring i went to a lot of therapist and chiropractors and people who massage alot. But i have this pain for over a year now and i am wondering if this wil ever heal i am even doing this now. After this exercise I feel no pain but after minutes the pain comes back what should i do. I even made a mri scan but they didnt saw anything.
Good article my symptoms to a T, just had cortisone injection into buttock today and the information in article was beneficial to me as to recovery, been troubled with it for over a year – a real pain in the butt
I am so thankful I found this article. I am an athlete, playing multiple sports year round. I recently tore my hamstring, around 3wks ago. The first week was pretty painful all throughout the hamstring to buttocks area, but over the past 2wks I have had serve local pain in my buttock only, the worst is when sitting. I am currently in therapy and they are treating the pain through ultrasound, stem and pain patches. I have found that rolling up a t-shirt and placing it under my high hamstring area close to my buttock when sitting relieves the pain.
I hope to start the above return to running routine within the next few days. I feel ready to run, but the pain when sitting is very intense. Thank you for the great article.
Hey i read about your injury in your hamstring.
I was wondering how it ended up going?
Im currently hurt for 3 months.
Im stil having struggles sitting. I also cant sprint and have difficulties doing physical activities.
Please let me know how your recovery went
Thank you
After six months of severe discomfort and disability, numerous physical therapy sessions, dry needling, massage, cortisone RICE, the kitchen sink, I had a prp injection. My immediate reaction was regression to more discomfort, however at the six week point I was significantly improved. At the 12 week point, I am virtually recovered.
My doctor, Jason DeLuigi, OD, Georgetown Hospital, Washington, D.C.
One more comment, especially to Jenny. I too could not sit for six months.
I urge you to consider a prp injection. I believe that I would not have healed had I not supplied the right healing components to this tissue which receives so little blood flow.
Remember, tendons are barely living tissue. That is why cadaver tendons can be use for transplantation. It is essential to get blood to flow into that tissue. If you have waited a long time, you could now be in a stalled healing and week tissue situation. The prp injection coupled with needle tenotomy will restart your healing and give the tissue what it needs to heal properly. Scrape together the thousand dollars it may require and have this effective treatment.
Marc, I just got PRP done on my high hamstring tendinopathy and I am about 3 weeks out with only a marginal sign of improvement from pre-PRP procedure. What triggered your recovery at the 6 week point? Did you do any cardio during that period (running, bike, elliptical, etc)
I look forward to your feedback.
Sorry for the delay Greg.
Nothing triggered the improvement I experience six weeks after prp. It just happened. I am now eight months post prp, and I continue to fetal better, though it is clear that I am not the same man. Deep tissue massage helps a lot. I believe I am left with adhesions and I adequately healed tissues. I am much much better, but I’m not recovered fully. Surgery seems risky, but I may consider that after another six months.
I also had a PRP injection about 4 months ago for high hamstring tendinopathy on the left side that I had had for 18 months. I had continued running during that period, backing off to spin and swim when it got too bad to run. It was uncomfortable sitting in the car but tolerable since I don’t spend much time in the car. Twice during the 18 months prior to the shot, it started causing changes in my gait and I ended up with some other running problems that made me completely stop running (posterior tibial tendonitis, for one, in the right foot) . So I had an MRI, which showed a partial tear in the common hamstring tendon.
Part of the motivation for the injection was that I couldn’t run at all, due to the PTT and the time on crutches would help heal that as well. It was painful to be on crutches with no activity for 2-3 weeks after the injection (at my doctor’s insistence) but it’s actually much better now, 4 months later. I can finally touch my toes with straight legs, and kick my shoe off with the other foot without pain.
It hasn’t been fully tested with my previous mileage, but I ran a few 7 milers with no problem, until I somehow managed in the past month (I think going too hard at spin class) to do the same thing to the other (right) side. And this time it is very painful to drive. I now have a cushion in the car and am very frustrated. I don’t know if I should just have another PRP and somehow get through the 2-3 weeks of inactivity, or how long to cross-train and see if it goes away on its own. I’m now doing much more glute strengthening and stretching than I was before, it makes me feel better if nothing else. I was running through it until 5 days ago, when it started bothering me 6 miles into a 7 mile run. Odd. But now it’s noticeable even a bit when walking.
I am writing in hopes this helps someone reading this thread. I am a 58 yr old distance runner. I had/have severe HHT for the past year to the point where I could not sit at my desk for 10 minutes and could not jog 1 mile at even 15 minute pace – I felt like my glute was ripping from my hamstring all the time. This was mostly up under my right buttock but also on the ischial tuberosity (sit bone). I believe I aggravated or tore the tendons by running hills too much and then over-stretching by touching my toes keeping the legs straight. (I know! Some people don’t get wiser with age!) Back in January, I read this article and a few others and decided to aggressively strengthen my abs and glutes. I do all the exercises listed here every day– bridges, planks, everthing– eventually adding in the swiss ball curls. I swim 2 – 3 times a week with laps of backstroke just using the legs and laps of kickboard. I use the glutes/hips machine in the gym 2 -3 times a week. I do have easy access to a gym and a pool so that helps. I also ride a stationary bike –standing on the pedals. I’m not sure that helped but I wasn’t sitting. Also ab work and clams with a stretchy band.
By March/April, I could sit for longer periods and the pain in my right side began to subside. BUT then it shifted over to the LEFT! Aggggh. However, the lessening on the right encouraged me to keep on fighting it and now I can do the back plank leg lifts with my left leg up with no pain. I can do one or two with the right leg up (left glute engaged) but that does cause some pain. I feel like the left is starting to lesson but occasionally does flare and burn down my hamstring. I can run 4 – 5 miles now at about 10:30 pace with dull pain on the left . I ran an 8 miler last week at 11:30 pace — no acute pain, just no speed. I also roll my legs–front, side, back–every night and do the leg stretches throughout the day. It is like a job and more time consuming than marathon training, but I am sticking with these exercises and feeling some results. I don’t know if this routine will work for everyone but I hope relief comes for you.
Hi John, thanks for reaching out, and we are so thankful for you sharing your improvements from using our suggested exercises. Hopefully it continues to improve, and your perseverance will pay off John. Those exercises will make you stronger, and less likely to suffer with this issue in the future. Is there anything else we can help you with? Others will take some comfort in your comment, and we really appreciate your support!
Am really glad I found this article. I have been suffering from the same symptoms for around 9 months. I go to the gym 5 times a week and do a lot of spinning, weight lifting and a bit of running, however the pain is only really bad when I am driving and sitting at my desk. Sometimes I have to stop the car and get out to stretch. I had an MRI scan two days ago and am awaiting the results in anticipation. It will be interesting to see what shows up.
What were the results of your MRI? Thanks, and I hope you are getting better. I have the same symptoms.
Hi,
I just developed this injury (or it became mroe apparent) after this last marathon on Nov. 10 where I could barely stand the 1 hr drive home and had to have my daughter take over.
question is – how is this diagnosed and if it is early enough in the injury, do I have hope that it will take less time to recover if I do not run and how long before I can run again. ANy hope for a spring marathon, which will require 16-18 weeks training starting mid-late Dec or early Jan??
I can relate to all these things. I am going to look into the prp needle. I did my injury in 2007 while teaching karate. It was bad for a long time. Sitting was the worse. I wish I had an MRI at that time but didn’t until 2013 when I felt the tendon snap again. I can now sit thanks to massage and Dr. Lowell Grieb. But when I start to run I get a little ways and start to limp again. I am doing isolate stretches for the hamstring and balancing on one foot. I do need to strengthen my core – major work there. It is a long process. If it hurts to sit, I would recommend not to run. Good article.
Have had this injury twice now, and ART really helped me a lot in getting back to being pain-free. Try it, and good luck to anyone who has this nasty injury.
My ? is, I just started running, Im 50 and started walk running only 1 month into it I started having this pain in my piriformis, I thought it was piriformis syndrome, but the xray and MRI showed lower back 3 disc compressed and 2 that where herniated sticking into spinal cord and arthritis in that area. So Ive been to get a massage just on my right leg and but area for an 1 ht every week and decompression. Ive been going this since Aug with no help. How do I know if I have this injury you are talking about
I am not a fan of cortisone shots or any treatment that is invasive. I treat with cold to keep inflammation down naturally. Although I treat a lot longer then just a few minutes here and there. There are some evenings I have a cold wrap on for 6 hours. A friend of mine depends on a Blood Flow Stimulation (BFST) wrap before runs. I have tried hers before but was not able to use it routinely enough to see an improvement. Apparently it just warms up the area without causing any additional strain. It seems like the pain will always be there but I am at least able to go about my day to day. Oh, and a good massage therapist who knows their stuff was a huge benefit as well.
Hi,
I finished a marathon on Nov. 10 and I knew I had some issues in my right leg. There is a strain in the innerside of my right foot which I went to a podiatrist and now going to PT and was casted for orthodics. I backed off running quite a bit in the past 20 days and have only ran a handful of times, and mostly easy from 3mi to 7 mi and I only did a turkey trot 5 mi at about 8;15mpm pace and then two long’ runs of ~7 mi. Now I think that I have this high-hamstring tendonitis – it sounds like everything you are talking about. I have a desk job and any travel in car more than ~30 min is painful and this past weekend traveling ~5 hrs to WI, was excruciating after ~3 hrs to the point that I had to have my 15 yr old daughter take over the rest of the way.
help? I contacted my podiatrist to see if he had a referral for the hamstring so that I could possibly get PT for both the foot and hamstring injury because I already am lacking time for the one PT. Also, I had been doing cycling more than running since the marathon because I thought it would be better for the foot; now I think I may have made the hamstring worse by doing this. What is the best alternative exercise for me – eliptical, treadmill inclined walk, and/or stepper??
Great stuff and a huge help. I esp appreciate the mix of hard citations and practical photos/application — very unique.
Could iodine and/or folic acid deficiency (and it’s impact on thyroid (>hypothyroid) be partially to blame for the inability for the high hamstring to recover? I ask because almost instantly after taking the supplements (for suspected iodine deficiency) I turned 100% normal in function for the first time in many months of battling sitting/butt pain. Besides that, I was 1.5 years into knee joint pain and nerve tingling sensations and leg muscle fatigue – all of which was on the mend 6 months after it began (and after bloodwork ruled out of some of the worst suspects – I had NO inflammation at all). So only now in the last 3 weeks, have I felt 100% in 1.5 years!! Knock on wood, I’m watching closely but even my runs have been spectacularly normal – such that I forgot how easy they used to be!! Prior to this supplement, I found B12 to also be a miracle cure to the muscle fatigue. Just wanted to throw it out there since I’m shocked by the dramatic improvement. Can’t see how it would be a coincidence that everything cleared up after taking the supplements (in a prenatal multivitamin actually).
I have been to three separate physical therapy clinics for my high hamstring injury; each time following all instructions and never missing an appointment. Finally, this article addresses my problem. More “core” exercises please.
Thank you!
I have had this for 1.5 years with little progress in resolving it. Mine came on suddenly whilst doing some seated twists with a medicine ball and feeling a ‘pop’.
Other than the soreness at the top of the hamstring, i have an associated symptom which i have been unable to find any information on or concrete answers from various physiotherapy professionals.
I get a ‘twang’ in my butt like a cord catching on something then slipping off/releasing. This happens when i do anything that stretches my hamstring beyond normal walking tension. I think it might be my sciatic nerve but i have no idea what it might be catching on. When it twangs it can also feel it behind my knee somewhat.
Anyone else have experience of this?
I’ve just had a Cortizone ‘wrap put around my tendon and am about to start out on a concerted rehab program, hopefully i can kick this once and for all.
I’ve had this three times over the last year (as in it’s recurred three times…) and in all honesty the best thing I did was go to the physiotherapist. After a week of muscle strengthening exercises I started to notice a difference and now my hamstring is almost completely better. I feel so much safer running on it, after it went the second and then the third times I’ve been living in a state of fear that it’s going to go again. It’s so subtle when it does but it doesn’t half take FORVER to go away.
Anyway, before spending loads of cash on an MRI or getting cortisone injections and so on, I would recommend just seeing a physio and seeing if they have any suggestions. For a number of reasons I was particularly stressing my hamstring which was also a lot weaker on the affected side. Probably because of all the downtime it’s had… still re-building it at the moment. I’m hoping to get it up as strong as the other before I try really testing it – sprinting, hill running etc.!
I have what I thought has been piriformis syndrome for about 4 years and I also refuse to stop looking for a fix. I am interested as my issue may be hamstring related and this caught my attention. I have been reading a lot about hips and shoulders, I have a book called Sitting, Standing and Walking and have purchased the corewalking program (corewalking.com). All of these are opening my eyes to the psoas and our posture/alignment. Much of our issues may be related to our slumping posture (I sit at work all day too). I have only started my changes with the walking techniques so I cannot say yet if they help, but I do notice that when I use no music and concentrate on my posture running that when my butt starts hurting on one side, I lift the core and release my body and that help. Main thing I’ve learned is how tight we keep our buttocks when we walk and surely when running. I am having a hard time walking with a loose butt but am going to keep trying! By altering your posture it helps. Also ensure the feet go straight – not out to the sides! This will come with walking upright since you can’t force your feet alone to change. I have not tried any stretches that help so I am doing somatics as well. Best of luck
I have had this injury for 20 years. I had a waterskiing accident and it tore my hamstrings severely. For sometime I went to PT. I had always been active…biking, jogging, weights & aerobics. I can do nothing in the way of exercise and my muscles have wasted away. It injured my S.I. too. Both legs went up over my shoulders.
I am now in daily pain and cannot get off of meds. I wish I had known about what you are detailing here. I’m so sick of this and the docs can’t give me injections more than twice a year.
It gets aggravated and I can’t sit for too long. Can’t ride, run.
Any hope?
I had this injury for about a year from doing sprints. This was the worst and most depressing thing ever, i coudnt run and i was always in constant pain. I must say corticosteroid injection & 2 sessions of ART fixed the problem. Now im pain and can run again!
I have had both Knee and Back Surgery’s like 12 and 13 years ago now. No total knee though, but my knee is shot and seems to shift when I walk. 2 years ago, I fell down our stairs, about 3 stairs only, my word the pain was so intense in this area you have described here. my doctor sent me for an MRI, I could not even get though it, due to the horrible spams. 3 months in a wheel chair, and prescription meds. It finally felt better until last week. This time I have done nothing such as falling, just up and down our stairs at home and standing on chairs lately, as we have been packing for an up coming move. I feel like a baby going to the ER with this pain, but it keeps me awake and hurts so bad. my reg doctor does not have any thoughts on this, since he not a specialist. I am no athlete, I’m 55, but my symptoms sound exactly as described here.
I have similar pain high in my hamstring near the connection to my sitz bones, but my physical therapist has diagnosed it differently. Pushing or massaging the tendon gives no pain or tenderness. Rather, I have had prolonged issues with my sciatic nerve passing through my piriformis muscle. It also is aggravated by sitting. My treatment is getting the hips aligned properly to get rid of the sciatic nerve irritation. Once I get that adjustment, my pain goes away. I use a standing desk and sit on a pillow when I need to sit.
It wasn’t until I had a high resolution 3 T MRI that I was diagnosed with two high grade near full thickness tears in both hamstrings at the point where the hamstrings attaches to the IT. For 15 years I was told I had one ‘small’ tear, but was never given any advice on how to treat it other than a little RICE, and because I had other seemingly more critical injuries at the time, treatment of my hamstrings were never a priority.
I cannot sit in a chair or drive for more than 10 -15 minutes due to excruciating sciatic nerve pain, and often while driving, I have to pull over. Recently, I had Proximal Tibial nerve and Common Peroneal nerve surgery on my calf to relieve nerve compression pain. This has helped the shooting, burning nerve pain in my calf. I was almost about to have my PFCN (Posterior Femoral Cutaneous Nerve) removed in one leg (my neuro-surgeon thinks that because it’s damaged from the hamstring tears, it’s causing the nerve pain when seated). I decided to see a hip and hamstring specialist first to see if the hamstring tears can be repaired. If they cannot, I will have the PFCN removed. The PFCN is a branch of the sciatic nerve that travels down over the lower part of the buttock and over the IT where the hamstring attaches.
I wish patients with this condition were treated more seriously, especially non-runners. In general, hamstring injuries are considered a ‘sports injury,’ and if you’re not an athlete (football, soccer, running, etc.), you aren’t taken seriously by orthopedic surgeons. I found this to be especially true as a slightly older female. Even though doctors knew I was a dancer, but they seemed unaware of how extremely athletic dance training is.
It is time providers address preventive hamstring care, and not simply tell patients to RICE. If you’re an athlete or dancer, you’re going to push yourself for the love of what you do. If you’re told it’s not serious and will heal with a little rest, you aren’t going to be aggressive about treatment or preventative care for the rest of your life. If we now know that the hamstring is fickle, easily re-injured, etc., let’s incorporate that knowledge into patient care.
Ms Burgess’ account of her ongoing quest for diagnosis and recovery has got to be one of the most depressing things I’ve read yet about this injury. I have had a hamstring overuse injury for about nine months now, finally diagnosed as high hamstring tendinitis, and have at this point not run for over three months. I never had an acute injury; rather, it was overuse during marathon training. In addition to having mid and high hamstring soreness I also have pain at the ischial tuberosity while sitting – as I must do five days a week for my desk job. I had about nine weeks of physical therapy but then saw another therapist who pointed out that most of the exercises I had been prescribed were working, rather than resting, the hamstring. Now I have started a completely different therapy regimen to address ‘sleeping glutes.’ While this explanation makes more sense to me, I’m not yet convinced that it’s helping any better than the other therapy. I have increasing concern that this is a condition that is just not going to go away. As for Ms Burgess, my loss of running is a significant one in my personal and emotional, as well as physical, well being. My activities are becoming increasingly more constrained. I have read repeatedly that little is known about this injury and how to treat it. I wish there was a more clear protocol for diagnosing and treating this problem.
I have been doing lots of research and I am convinced this is what I have. I can’t pinpoint the exact moment the injury occured but this has been going on since February. So 5 months now. I am 53. I do a bit of running but I think the injury must have happened playing hockey.
Like many that left some comments I cannot sit comfortably. Working at the office and driving are the worst. It`s literally a pain in the butt. Sometimes radiating down to the side of the knee. When I avoid sitting the pain goes away somewhat.
I do core exercises and leg strenghning. I will add the exercises mentioned. I am never sure if I should rest or keep exercising.This is really making my life miserable. I would like to avoid the cortisone shot as some say it only heals temporarily.
Great article – thank you. I’ve just today injured myself (severely) with this high hamstring injury playing competitive indoor cricket. Will describe my history more later and post my rehab and recovery notes.
I’m a multi-sport athlete and damaged my right hamstring doing a deep split (which I had never-ever had any problems with). I have had pain off and on for about 2 years now when I tweak it or sharply increase my training load. Core strengthening, yin yoga and self myofascial releases have been VERY helpful! Yin has been absolutely transformative for my body (not just my high-hammy injury)..yin involves working the soft, connective tissue and fibers… I highly suggest attending a class and make use of the props- let your body settle in and hold for time- WOW!
I want to cry. I think this is exactly what I have and I have been in denial. I’ve been doing a lot of these exercises, but I’ve also been trying to run through it and it is only getting worse. I have all these races coming up and I probably shouldn’t even be running. I am so sad
I’ve had this for about 5 years now. I injured my hamstring while running. Went to see a PT who made it worse, so that it hurt to sit. Now I have pain on both sides, and it’s torture to sit through meetings, drive for more than an hour, etc. I don’t even try to run anymore. I’ve had steroid injections on both sides twice, PRP on both sides TWICE – and they did help for several months, but the pain returned. And the physiatrist basically gave up on me after that. Went to see another doctor, who did an sacroiliac joint injection, and that didn’t really help. Have been in PT on/off the entire time. I’m so tired of hurting. And no one has given me a clear diagnosis. I walk around with cushions to sit on, and I’ve actually decided not to pursue a graduate degree because I don’t think I can handle sitting at a computer or in a classroom. It’s just crazy.
This article and the essay by Ms. Burgess resonate so strongly for me. My story began in March 2013 when I was training for a half-marathon. I, too, blame overtraining and lack of strength training and cross-training for my injuries. It started with tweaking on the inside of my left ankle which ran up and across my left knee – that took me out for a couple weeks. Shortly after resuming training – and hill repeats – the backs of my legs were strung so tight from my gluts through my plantar fascia that I could barely move. This eventually led to a sudden tearing in my right Achilles, which actually provided some relief but simultaneously caused tremendous havoc. I was forced to sit even more than usual (I also have a desk job) and I compensated for the injury with my left side. It wasn’t long before a hamstring strain on my left side led to high hamstring tendonitis, ishial tuberosity bursitis, and finally troncheric bursitis. I couldn’t sit, stand, lie down or walk without significant difficulty and pain. I had to stop working for 8 weeks and then returned to a sit-stand work station at which I am yet to be able to sit. It’s now been 7 months and I’m still unable to sit down for a meal, go to a restaurant, go to a movie theatre, or drive in the car for more than 5 or 10 minutes – let alone run. It affects every area of my life. The time when I’m not working is spent trying to heal enough so that I can continue working. I feel like I’m caught in a vicious cycle. I’ve tried PT, massage therapy, cranial sacral therapy, holistic nutrition, yin yoga, swimming, cortisone, ultrasound, RICE, etc. Now I’m getting an MRI and going to try shockwave therapy, and if that doesn’t work, more cortisone. If I don’t have any success, I will seriously consider surgery. I am desperate to get my life back. I would be interested in hearing from others with similar challenges and welcome any advice or recommendations on treatment options.
I’m in pain. I have done spinning class for a few years. This year I have slacked in working out and regular excercise. I had not done spin class’s in a month and decided to get back at it. I did a 1 hour advanced hip hop spin class on last Saturday a fairly moderate class Monday. I noticed even with my gel seat cover the seat hurt. By Wednesdaymy legs felt like workout pain but wasn’t too bad. Thursday I started feeling pain under my right buttock. Now it is bad, it hurts to sit,get up bend down, and stretching is out of the question. I believe it’s the hamstring. What can I do for this??
Thank you, thank you to author of this article and to everyone who is posting. I have been suffering through this for 2 1/2 to 3 years now; I am not a runner, but exercise regularly. I received accurate diagnosis only about a year ago. For the first nearly 2 years, orthopedic doctor was baffled – I had x-rays, steroid injections, SPECT scans, MRIs, etc. The bone SPECT scan combined with the MRI finally pinpointed the high hamstring tendinopathy. Tried physical therapy last year, but it didn’t help. Sitting is the worst. I have a sit/stand desk at work, which helps, but my hour commute in the car twice a day is an absolute killer. I end up standing in the back of a movie theater halfway through the movie because I can’t sit that long. I stand at the end of a nice dinner, because everyone wants to stay and visit and have coffee/dessert, but I can’t sit that long. Doctor says surgery is out of the question for me, so going back to physical therapy to try again, but if that doesn’t work, maybe next step is PRP. Thanks again to everyone who posted. We’re all in this together.
Wow…! Thanks for the article and thanks to all that have posted and provided info. I never reply to anything like this, but since the origination of my experience with this pain in the a** – sounds a bit different-thought I would. I first experienced these symptoms rowing crew in College in the late 70’s. Like many of you, sitting in the car or straight up on a bench was very painful, but I ignored it. After college I had a long career in triathlon and cycling which included a lot running including power/speed/agility drills, stairs and marathons. Quick accelerations/sprints/bounding were the worst. I managed it with weight and core workout and then added yoga in 2002 which helped tremendously. But with yoga, particularly heated yoga, I tended to overstretch, but didn’t pay attention to the fact that pain is a messenger. I finally quit running in 2007. Since, I still compete at a high level as a cyclist, which does NOT aggravate this area the way lifting, stretching or yoga can-which probably has more to do with me being to aggressive or not listening to the pain/inflammation. Two weeks ago I sat back down on a rowing machine to prepare for a race in November and BAMM!! In the first minute I felt like I was rolling up and over hot, inflamed cords with my sit bones and after only 3 days of attempted rowing for 20 minutes – I’m toast and now searching for help and reading this article. Think I’m going to go sit on some ice. Best to you all!
If you have this type of injury for a long time and you are in an older age group which makes it difficult to fix and are getting no improvement speaking as someone who did everything over two years physio programs x 2, steroids orally and injected, glucose injections and 3 PRPs get an MRI! It showed in my case the tendon and completely separated from the bone and surgery was the only option. it won’t be the case for everyone and surgery is not always an option. I have had surgery and it is a slow road back. Take care and good luck!
Good luck also to you Karen. I too have had surgery. It is a very long, very slow road back, but it is worth it. Every day every slow run, it is worth it. Not one day since surgery have I regretted finally having surgery. I just wish I had acted earlier. Saw someone that specialising in this horrible injury earlier, and had surgery sooner. But I have done it now. 17 months since surgery, and I am so thankful to my surgeon. I sincerely wish you all the best in your future running career.
Hi Karen,
How are things going with you since your post on the 04.10.14.? I hope that you are continuing to improve. Reading some posts are quite distressing, and I hope these athletes find the solution they need. There is hope from this injury, and I look forward to hearing how you are going.
Lynn
Was diagnosed with upper hamstring tendinitis on my left side about a year and a half ago. I went to pt and began running in about 3 weeks again. Off and on it has been bothering me mostly just when I run. I have been doing core strength training for about 3 years and I believe that it has helped. Just recently it has acted up again and I received a cortisone injection my first in 60 years of sports. It did not help. I have no pain while driving or sitting. Rolling it with a small ball gives u a nice deep tissue massage and helps reduce the scar tissue. Biking is fine and also elliptical machine. I am going to take a couple of months off from running,very difficult since it is very enjoyable for me. Heat in the morning when I wake up and ice before I go to bed seems to really help.
I was diagnosed with proximal hamstring tendonitis about two months ago. I began experiencing pain/soreness/discomfort about 4 months ago. I’m now going to physical therapy and am on my 11th week of not being able to run. I am a runner and was typically running 20-25 miles a week. I believe that I gave myself the injury by using the hamstring curl at the gym… It gave me some micro tears in the tendon and then I continued running on it for a little over a month before giving in to the fact that I was dealing with more than just soreness and something was wrong. I was not very good about stretching my hamstring before this. This article sums up my experience in many ways. Not being able to sit for more than an hour without pain & stiffness and a frustratingly slow healing process. The PT doesn’t seem to be helping very much. At times, it has been very depressing because cycling and even swimming hurt so all I’m left with is walking. For a runner, this feels devastating. I’m so grateful to find this article and read the comments. I haven’t tried cortisone injections yet, although I’m now thinking it may be necessary to give it a try.
Heather, you sound exactly like me. I was running a lot, but I think adding in too many hamstring weight exercises (like curls and squats, etc.) caused microtears. I continued running through the pain and eventually got to the point I couldn’t run. After resting the injury (not running at all) for 3 months, it was still no better. I went through 4 weeks of PT…with no improvement. Saw Ortho Doc and MRI confirmed high hamstring tendonopathy. I just finished up my first PRP injection (4 weeks out) and tomorrow I go for my 2nd one. I’ve seen a little improvement…but definitely not enough to even think about running. Still hurts to sit for any longer than 30min. I’ve heard that if PRP doesn’t work, a tenotomy could help. Hope your hammy is feeling better! Hopefully I’ll have good news in the next month or so after the 2nd injection and more PT!
Hi Shannon, sorry to hear about all the trouble you are having with your hamstring. Hopefully the injection will give you some time to allow it to heal. Have you tried Active Release Therapy to loosen the muscles around it? Keep us updated with how it is going! Best of luck!
Hi Shannon S,
I’m wondering if you could update me on how you’re doing? I got my first PRP treatment a little over two weeks ago and have had no improvement. I’m thinking I’ll wait another few weeks before getting another one but if you could tell me how you’ve progressed that would be really helpful. Thank you very much!
Monica
Oh, my heart goes out to you all! Thank you for sharing, it is so good to know I am not alone. I have been battling this pain in the butt (literally) injury for seven months and have tried physio, regular (weekly) deep massage, chiro, acupuncture, glute and core strengthening, specific stretching exercises, yoga, Bowen therapy, Ortho-bionomy and rest – pretty much all at the same time and for prolonged periods, but nothing seems to help permanently. Apart from being frustrating, and time consuming doing all the exercises, it is costing me a fortune!! From what I read here there does not appear to be any reliable treatment or cure. Very depressing – and suprising. Surely, with all the advanced medical and alternative therapies out there someone has the answer. Like many of you, sitting – at my desk and particularly in a car – can be excruciating. And like most of you I am pretty desperate and would do just about anything to find some permanent relief. I’m sorry I can’t offer any suggestions for a wonderful solution myself but it seems the best course of action for me is to run less – less distance, less intensity – and swim, cycle and walk more. I find if I take anti-inflamatory tablets a few hours before I run I don’t get nearly as sore either during, or after the run. Obviously, however, this is not a great practice to get into as anti-inflamatories can mask warning pain and should not be taken as a long term solution. I empathise with you all and am grateful to have found this article and to hear your similar stories. Good luck!
Thanks for the article and now the associated ‘support group’ for people with this condition. I have been struggling with this for 9 months which seems an eternity but a blip compared to some of the stories here. I am a PE teacher and a CrossFit affiliate owner and I can do any and all exercises without pain. Deadlift heavy, squat full ROM, toes to bar, you name it – no problem, BUT put me in the drivers seat of a car and in 15 mins I am in agony. With a lacrosse ball under the high hamstring I can get a squirmy one hour drive accomplished but it is extremely frustrating and impacts life considerably. Has anyone had any success with Rolfing? I intend to start soon now I have exhausted 3 separate treatment practitioners without any improvement whatsoever.
Sorry to hear that James, but sounds like you are at least able to do all the exercises that will strengthen the muscles around it. I actually am going through this myself right now, so I understand what you are saying! Hopefully some of the other readers will be able to give you their experiences with Rolfing, myself, I have found that ART is great, and actually the kinesio/mcconnell tape works quite well. Hope this helps, and hopefully it continues to get better for you!
I am a personal trainer. I injured myself after working out last Friday. Saturday morning I was in a lot of pain, as some of you have accurately described a real pain in the butt. Wow. I stayed off my feet Sat and Sun. Monday I was no better. That is when i found this blog. It is very informative and I took notes on what exercises and stretches that i could implement. Yesterday I stopped by the gym to talk to the owner. He works with a lot of athletes. Of all the people I know I thought he would have bumped into our shared pain in the butt (high hip tendinopathy). He handed me a tool, he use on some of his athletes. It is a metal device called a DMS, Deep Muscle Stimulator. He said To turn it on and rum it on the back of my leg. It took a minute to get use to but then I got more comfortable with it. I rubbed it on my hamstring for several minutes. It felt like the hamstring was warm, he said it was increased circulation. It took about half of the pain away. I still babied it. I went to the gym this morning and used it again. The muscle felt a lot less tender than yesterday. I then drove to my job using a pillow under my hamstring just to be safe. I sat through a two hour conference call, no pillow and then drove home, which is an hour away from my home. My condition feels much improved. My hamstring still feels like it could flare up, so I am not pushing it yet.
The owner of the gym where i work out described what I have as a muscle that had contracted and when it did it pulled on the point of origin, the iscial tuberosity. That was why it was so point tender. By using the DMS to relax the muscle it could then release the tension I was feeling at that point of origin. It is probably not easy to find. Google it or if you are close to The Lake Geneva area of Wisconsin, I would be more than happy to show you. Good luck, I am very grateful to have stumbled onto this solution.
Interesting Bob, glad to hear that worked for you. Hopefully yours continues to improve. Some of the other readers will likely find this information very helpful, and is definitely worth a try if they can find it. Thank you for the input!
I have had a high hamstring injury for nearly two years now, and it is the most depressing condition. Mine happened after five years of long distance triathlon (and turning 40) and trying to get quicker. There was no tear or pull, just a gradual on set after running. My biggest mistake was trying to stretch it out, this made the condition immeasurably worse. Forward bends and hamstring stretching are a big no for me. So – after nearly two years – I have had two MRI’s to confirm the condition, tried three physio therapists, had shockwave therapy, two corticosteroid injections, massage and chiro. I’m stillnot really ‘healing’ but I have learnt to adjust my life to fit the condition. That is what makes this such a big deal. It beats you down. I cant run, cant bike, cant sit through a movie or a meal, cant drive long distance, cant concentrate through long meetings… the list goes on. But I can swim, I can feel that rest helps, and I have hope that by adjusting my life to cater to this condition I will eventually get better. BTW the shockwave might be worth trying as for me it really changrd the nature of the injury, it moved the location of the pain, which I’m told is a good sign.
Hi Matt, sorry to hear of your struggles with this. Hopefully reading some of the other reports from others can provide you some comfort as others are going through a similar struggle. We are glad you are slowly becoming at peace with your hamstring, and it is good you can still swim with it, that will allow you to gain some fitness. If you find anything else that helps, we would be interested to hear, as you may help others before theirs becomes chronic.
I have had this problem for over a year. I have had a PRP and have gone to physical therapy at a couple of different places. They all prescribed these exercises and they did NOT work.
The big problem, however, is that (from physical therapy 2-3 years ago) found out my pelvis is mis-aligned, and is the root of the hamstring tendinitis. I used to have tendinitis on my other leg on my patella tendon. Now, the injury has manifested itself on the hamstring on the other side.
AFTER i have corrected my pelvis alignment I started doing these exercises and they have helped a lot.
You may want to speak to your doc about alignment issues.
Good luck!
Thats great Bob! Glad you are feeling better, alignment is a huge part of preventing hamstring pain, especially if your pelvis is tilted. Good to think about though, and we appreciate your input.
i have this injury as well and have been dealing with it for a year and a half. These posts have been depressing and gives me a feeling of despair. I don’t care if I run – I just want to exercise and remain fit. I have severe scoliosis and am wondering and am sure that causes misalignment. Has anyone had this combo and is it possible to improve pelvic alignment without having scoliosis surgery. I am trying to avoid scoliosis surgery as I am 63 years old. I feel very discouraged. I got a cortisone shot with guided ultrasound and it made it worse, not better. Any targeted suggestions would be helpful as the suggestions are overwhelming me – rolfing, pelvic alignment, core and glut exercises, rest or not rest, mri, surgery, ART and gastron. I don’t know where to start.
Hi Meg, sorry to hear that. You will enjoy our posts this week, as they are focused around being able to run well into your older years. I agree that you do need to heal up this hamstring, but it will heal if you are doing the right strengthening exercises to allow it to do so. Did you sign up with our newsletter on this page where it says about downloading the full recovery and prevention routine? You can get more information about high hamstring tendinopathy, and the methods in that are worth a try. We want to help! 🙂 Make sure you check out our podcast tomorrow with Kathy Martin, she will inspire you, as will our interview with Maragaret Webb in a few weeks! Hope this was at least somewhat of a help!
I’m somewhere at the beginning of the HHT fever dream. Used to be a runner until training for a marathon landed me in knee surgery (6 yrs ago). Went back to dance about 6 months ago in preparation for an audition that’s now about 2 months away.
But in the beginning of Nov. I got hit with the HHT stick.
MRI confirms slight tear/fraying.
I stopped dancing entirely to let it heal but it just hasn’t.
Every PT I’ve met says “steroid injections” are the answer.
Now I’ve met with 2 different orthos who both looked at me like “say what?”. One recommends oral steroids, the other says PRP.
I’m scared of the orals – it just seems like sending a little steroid through my whole body is less helpful than a bigger dose right into the area. (Plus, I’m scared of the whole ‘weight gain’/’puffy face’ side effect. Now only for vanity’s sake, but as a dancer – you kind of can’t be “puffy”. Anywhere.)
However, the doc recommending the oral steroids says he’s against the shots because they’ll significantly weaken the area around the issue, then I’ll go back to training and rip the tendons right off the bone. Which is more TERRIFYING than being puffy. (and that’s saying a LOT – ha).
I’m fine with the doc recommending PRP, but they don’t seem to do anything for pain in the short term. And while 4 weeks of healing are perfectly fine (even great) under normal circumstances, at this point I just don’t have the four weeks to give.
The worst part is that I don’t know exactly how this happened so I don’t know how to keep it from happening again. And I can’t get any answers on “what I should definitely NOT do”.
It’s just so frustratingly confusing.
Sorry to hear that Liz, it can be difficult to know what information to trust, but the best advice we can give us just to trust your gut feeling, and listen to your body. You know your body better than anyone else, so you know what would be better for you. Hopefully some of the other comments brought you some comfort as you can see others are struggling also. Hopefully you find your solution soon!
This is my status update. I wrote a post 2 months ago. I have had no more pain or cramping in my high hamstring area. I used the DMS several times to see that the symptoms would not comeback. I read every post in this blog. The posts were pretty depressing. I was hearing people say that they had been dealing with this for 9 months to 3 years. Some had very little relief. I am very grateful that i bumped into the right person. For more info google DMS Deep Muscle Stimulator.
Wow. I’ve just been forwarded this article by a friend. I tore my hamstring (MRI stated severe) last April 2014! I’ve been dealing with it since. I tried p.t. then Graston Technique with no results. I am currently set up for four rounds of PRP. I had my first round early jan. I can identify with others regarding the ischial Tuberosity issue. I too have been dealing with sitting pain for ten months now. I will never sit on a wood chair and will sit on my coat if needed. Sitting is truly the worst and I have to sit for my job. I also find as the article states it’s easy to tear other glute muscles while dealing with this. Anyhow it was good to read I’m not alone in this! I plan to update this in the future especially when I’m finished the prp to detail results. I will not be finished treatment until July 1 2015. Here goes another half year of minimal lower body exercise and cardio. It is very frustrating but I am hoping the PRP is a success.
Thanks for sharing Caryn, glad you were able to find some comfort from the article and the discussion. If we can do anything else to help, let us know. Best of luck!
I have had this pain in the butt for over 5 years. I’ve had SI injections, trigger point injections in the glutes, cortisone injections into the bursa and quadratus femoris. I’ve recently been diagnosed with ischial femoral impingement and am going to a physical therapist to treat this. (Previously went to another PT for SI and piriformis which did not help). Last week the PT suggested that I may have high hamstring tendinopathy. The ortho doc agreed that this could be a conributing factor and suggested PRP. At this point, I will try anything that might alleviate the pain.
I am so excited to find this article as so much of it seems relevant to my situation. I do have a pelvic tilt and can’t seem to get across to the ortho doc or physical therapist that it may contibute to my pain. The physical therapist did start me on eccentric exercises for the hamstring last week. Since I’ve had this pain in the butt for so many years, I think that I now have a lot of areas that are involved since I have been sitting, standing, walking and laying. in incorrect postures. My pain starts in the low back in the morning and moves to the hamstring as the day progresses.
Thanks for the article and the comments. Many of you have described my daily pain.
Glad you were able to find some comfort through the empathy of others. Hopefully you find improvements, or one of the suggestions from the other readers in the discussion will give you an idea that will work. It is frustrating, but it is worth trying some of these alternatives.
Bob – I would love to try the DMS. I have been foam rolling my hamstrings and glutes to try and get the muscles to relax. I’m told that stretching is a bad idea because it adds further strain and compounds the problem. I feel like the muscles are constantly knotted up and if I can solve that issue I could get some relief. Lake Geneva is a bit of a drive, but after struggling with this the past 6 months, I would drive much farther for hopes of relief. I’m still very active and I completed a marathon with this condition in November, I’m just tired of the constant pain in the butt this is! I see my Chiro regularly, have been going to PT, and have done dry needling all with little to no improvement.
Has anyone tried PRP on hamstring tears? I am curious to know how they work on chronic tears. I have read encouraging research on acute hamstring tears, but nothing on older injuries.
I have had several high grade high hamstring tears in both legs – confirmed by MRI for over 13 years. One tear in particular right next to the ichial tuberosity is so significant two doctors said they’d never seen anything like it before – not something a patient wants to hear. It causes terrible sciatic pain whenever I sit for extended periods. I have had two MR-guided cortisone injections, which did not work. I have had dry needling (also did not work), accupuncture, massage and PT on and off for 8 years. My situation is complicated by severe hip joint arthropathy, a labrel tear and severe lumbar facet arthritis.
I have been told I need a hip replacement on the same side and was seriously considering the hamstring surgery first when I decided to give PRP therapy a try. I had my first round of injections (hamstring, hip, lumbar, shoulder and neck) a couple of weeks ago and am scheduled for my 2nd round in a week. So far, I feel acute inflammation around the left hamstring tear, which was expected as my body is healing. I have read that if it works to expect improvement some weeks after the 2nd injection. I wonder if I may need a 3rd due to the chronic nature of my injury.
Has anyone had experience with PRP?
.
Hi Gaby, we cannot answer for any of our readers, and hopefully anyone who has had success with it will reach out to you, but this article may help https://runnersconnect.net/running-injury-prevention/can-prp-injection-effectively-treat-chronic-running-injuries/
Hope you get it taken care of. If we can help, let us know!
This is definitely what I have. I’m pretty sure I injured it doing sprints a few months ago. It’s pretty consistent now as far as the spasms. Most of my pain is from sitting than running. I have a half marathon that I’m scheduled to run in 2 weeks. Am I making a big mistake by continuing to run to get through this marathon?
Sorry to hear that Jenn. Sitting is often the bigger issue, and hopefully you have found some comfort in the suggestions from others. You will probably be fine to race the half marathon if most your pain is from sitting, just be very careful with your speed until you know it is okay. Try to ease into the run slowly, and warm up well. Best of luck!
I’ve been dealing with left HHT since ’06, could not run for 2 months after the onset of the HHT and when I started back up my running form has never been the same. I have no pain but there is an upper tightness there, scar tissue that affects my running gait after approximately 4 miles into the run. Some times I pull over and stretch out my left hamstring which provides temporary relief to the my running form. Really hard to do long runs with this. It is like the left hamstring get’s weaker into the run and cannot do it’s job and it just along for the ride. I sit on a lacrosse ball to focus on the scar tissue that is still there but don’t really know if it is helping.
Hi Sean, sorry to hear that. Thanks for sharing what you have experienced, and some of the little comforts that have made it a little less painful. Hopefully some of the comments in here will provide you some encouragement.
I last made an entry above regarding my MRI of severe hamstring tear this past Feb. To re-state my condition, I had three opinions on my MRI, one being Ischial Tuberosity. I’ve suffered from chronic butt pain since injuring my hamstring Apr 2014. I had my second round of PRP mid Feb after my last entry above. This round included fat cells. I can honestly say I am experiencing windows of relief or some pain free hours post round two of PRP. I am able to do elliptical work and light leg weight work in the gym at this point with no aggravation or pain. My condition is by no means gone entirely. I still have trouble sitting at work all day although it is a little better. I still cannot sit on a wood chair without a pillow or even a jacket to cushion the pain but I can say I have hope at this point. This is just an update. My third PRP is Apr. I am hoping my last. I will update again.
Hi Caryn, thanks for reporting back to us, and we are happy to hear that you have some relief from the PRP, we actually wrote about it here https://runnersconnect.net/running-injury-prevention/can-prp-injection-effectively-treat-chronic-running-injuries/ which you may agree with the findings. Thank you for sharing, this will give some hope to other readers. Hope the third one goes well, and please, update us again!
A good explanation of what I think I have. Last Sept I started cycling again and did some big gear training, it was obviously to soon to ramp it up so hard as the next day I had upper hamstring pain. Not knowing what it was or how serious it could be I just had some massages (which helped) then tried to cycle as hard as I did earlier. In hindsight I should have stopped and progressed into your suggested exercises. I’m now on a merry-go-round of improvement and setbacks. I also have left hip stability problems and (as I’m finding out) weak core muscles. Was this article written for me?!!
Thanks for the info and I will certainly be talking to my physio about the exercises you have suggested and bring it into my daily rehab.
cheers.
Hi Paul, sorry to hear that. We did write this article just for you….all the other readers are just waiting for you 😉 Just kidding, but we are glad you were able to find some comfort in it. Please let us know how you get on! Good luck!
I’m not sure if I have this, I was doing circuit training 3 times a week and also spinning twice. After 6 months of doing this I got what I thought was a normal hamstring pain so rested, after a while I then got pain in the buttock on the left side so I went to see osteopath. We eventually came up with diagnosis of ischial bursitis so he sent me to doctor to get Naproxen, I have just finished three weeks of this and its much better but there is still occasional things going on in the hamstring area, I have no problem sitting anymore. I’m just starting another 3 weeks of Naproxen as I’m hoping this may keep improving the condition. No one on this thread mentions anti inflammatory drugs which I thought was a bot strange? I will update my condition in the next few weeks. May get an MRI soon though.
Hi Steve, sorry to hear about your pain. We are not really a big fan of anti-inflammatories, you can learn more in our post here: https://runnersconnect.net/running-injury-prevention/ibuprofen-and-running/. We do however recommend healing foods to promote recovery: https://runnersconnect.net/running-nutrition-articles/diet-for-injured-runner/ If we can help with anything else, please let us know!
I’ve suffered with H.H.T. for three years now. I was a runner with a desk job.
Due to this injury, I now no longer run or have a job. In fact, I haven’t sat down for over a year and a half. I realised the medical profession weren’t helping and I was going to have to help myself. Every time I saw a doctor they made it worse.
I’ve tried most treatments (steroid injections – which I regret, ultrasound, IMS – dry needling, eccentric exercise, massage, ART, Trigger Point foam rolling, Trigger Point ball rolling, serrapeptase to eat scar tissue, kenisio taping, hydrotherapy etc,) and read many research papers.
To help prevent this potentially life changing injury happening to other people and to help support those that have it, I’ve set up a Facebook page documenting my story, my mistakes, what’s helped and what hasn’t helped.
https://www.facebook.com/HigherHamstringTendinopathy?ref=aymt_homepage_panel
It’s only a support page to help and is not a substitute for advice from a good sports physio therapist.
Thank you Coach Tina.
Hi Vicki, sorry to hear that, thank you for sharing your story, and for providing a place for others to find comfort. We will leave the link for others to click on. If you provide a link to this post somewhere on your page, it will probably help the likelihood of it being found because of the connections within search engines. Thanks for sharing.
I have the same problem with high hamstring tendonopathy, and am planning to try these thin insoles (https://mortonsfoot.3dcartstores.com/) that are similar to ones I used to cure plantar fasciitis quite a few years ago. After trying all sorts of insoles and devices that didn’t work, these flat insoles helped me correct my over-pronation. They lift under the pad of the big toe, but provide no arch support. The doctors on this website think arch support further weakens arches and worsens the problems long term. The big toe lift triggers muscle reaction earlier than without the lift, and causes you to strengthen all the muscles that are weak and causing over-pronation. For a week or so, when I first started with them in both shoes, the PF side of my body was sore from neck through back through legs as my muscles were correcting themselves On the other side, they were not sore, because I was using these muscles correctly before using the insoles. It took only a month to cure my PF, after going a year with pain and trying useless remedies. Then I stopped wearing them, and my PF has not come back for years.
SO, I’m thinking that the same over-pronation could be causing the misalignment that causes this high hamstring tendonopathy. The insole website describes quite a few pain problems that are caused by over-pronation, so I thought I’d give it a shot, as nothing else seems to help. I’ve ordered new ones from the website.
Meanwhile, I was wondering if anyone else had tried something similar? It seems that strengthening the bad hip and gluts could help re-engage necessary muscles for correcting this, but if something in the way we run or walk, like over-pronation, causes the problem in the first place, we should work to correct it, too. Any thoughts or experience with such?
Hi Gina, thanks for sharing, and hopefully you found some comfort in the discussion from others. We definitely recommend strengthening your hips and glutes and we have a great post on how to do just that: https://runnersconnect.net/running-training-articles/hips-hamstrings-and-glues-are-the-key-to-running-faster/
As for the way we run, take a listen to this podcast, it should answer your questions, and you will enjoy what our expert has to say https://runnersconnect.net/rc43 Hope this helps!
Update: I’ve worn the inserts for a couple of weeks now, and it seems to be helping. I no longer feel a constant irritation, and even when directly stretching the hamstring with knee bent (which used to cause shooting pain), it is only a mild pain. I have been continuing my running and walking, which is mild compared to most runners on this forum. I run 3 miles 3 or 4 times per week at around a 12 minute mile, then walk on the off days. This is what I was running before using the inserts, too. Now, the running doesn’t exacerbate the pain afterward and into the night as it used to. Walking and running feels as if it’s building up muscles on the sides and front of my lower right leg (the injured side), and on the side of my right buttock. Walking seems to build different muscles than running, as different ones are sore after a walk or run. One muscle in the buttock felt sharply tight, as if it’s new to exercises, at first, but is maybe getting stronger and used to the new situation. I plan to continue using the inserts to see if it will completely heal this problem.
Hi Gina, thanks for the update, glad you are finding the exercises are helping you and you are able to return to running gradually. Being smart about your return like you are will pay off, and you will appreciate your runs so much more after all this. Thank you for sharing! Let us know if we can help with anything else.
So glad I stumbled on this article!! My initial injury happened with a rotational fall off a horse. Left foot was still in the stirrup when my body (right side) hit the ground – so I was “yanked” pretty good. I have been saying a million times to the chiro and the PT’s I work with “It hurts on the lift part of my stride” “right at my ischial tuberosity” and I get blank stares. I knew something was wrong when in lab, my partner muscle tested my L glute and I was a 3+ :/
I have enjoyed a few years injury free but re-irritated/injured it this past weekend. I’m bummed, but glad I found this, will be showing it to my chiro and PT friends! Thank you!!
Hi Rhonda, thanks for the comment. Sorry to hear about your pain, glad you found this post comforting, and hopefully our advice will help you heal a little faster. Let us know if we can do anything else to help!
A very useful article. I too am a sufferer (confirmed by MRI). I’m a recreational runner (or was) and keen dancer and dance teacher. I haven’t run properly since the end of 2013. The original injury was dance-related, landing from a jump in mid-2012. Stupidly I kept up my activities, thinking it would gradually get better, instead it went slowly downhill until I could no longer run a step!
Treatment: multiple attempts at shockwave therapy (unsuccessful); 2 PRP injections (they’ve helped a lot but not totally cleared it); physiotherapy (massage and rehab exercises); rest.
My feedback – PRP is worthwhile but expect to see improvement at 6-8 week mark, not early on. Sitting is hell and very hard to avoid. Return to activity must be very gradual (baby steps, people). And unfortunately, the injury seems to flare again for no reason (my latest flare up has coincided with a nasty cold – really strange). Oh, and wait until the day after activity to gauge how the tendon has reacted – there’s a delay in the process.
After a 4 month complete layoff I have managed to return to dance carrying frequent but manageable pain. I’m still trying to return to running due to frequent setbacks, other injuries (yeah thanks, calves) and illnesses. My dream remains of being able to run again pain free…one day.
Hi Jayne, thanks for reaching out. Sorry to hear about your trouble with your hamstring, it can be a very frustrating injury, and one that takes a very long time to heal. Thanks for sharing your experiences, this may bring comfort to other runners, great advice here, and shows an emphasis on listening to your body, which helps a lot. Hopefully you continue to improve. Is there anything we can help with with regards to your other issues during your return to running? (I promise it will not take me as long to respond this time 🙂 )
Well I certainly wasn’t expecting this much information at one time..wow..ok..I am however happy to see so much feedback as I find this is where you usually find some form of help..and it has a name..story of injury to come later..love all yall..
Hi, can anyone tell me how to sit comfortably on long car journeys (or even short for that matter) with hamstring tendinopathy? Ive tried a cushion but it only helps for a short time. Also, would icing it help to heal? Thanks
Hi Annika, your best bet is to try the suggestions of other runners in the discussion on this post. Quite a few runners have had the same problem, and some found relief. Hopefully this helps! Icing is not really going to help healing, your best bet would be to follow our recommendations in this post if you really want it to go away. Hope that helps!
Annika – I have dealing with high hamstring tendonapathy for about 1.5 yrs now, and have just discovered in the last month (slow learner) the secret to sitting for long periods, particularly in the car. I am going to post a more well thought out post in the near future, but this sitting thing is the only REAL partial answer I can offer. Last caveat – everyone has their own situation, so all I can say is that this has been hugely helpful for me. Bottom line when sitting, I had to remove the pressure on the sits bone/hamstring junction. Like you mentioned, a cushion sort of works for a bit, but after 30-60 min, the pain comes back. So I shopped the web for a cushion with depressions for the sits bones, but I couldn’t find one. I did see medical grade air cushions, but very expensive. So I had a soft, but dense foam stadium seat pad about 1.5 inches thick – sort of memory like foam – cost me 2 bucks. I sat on it while sitting in my car, felt where the 2 sits bones poked into it, marked the spots with a marker, then cut out a circle of the foam (all the way through) about 3 inches in diameter. Sitting on it sort keeps the direct pressure off of the sits bones. Last week, I added another cushion (identical to the first) but with a larger (about 5 inch) hole cut for each sit bone. I rode in the car this past weekend for 10 hours – no problem. It’s a MIRACLE!!!!!!! Positioning the cushions is sort of a pain, but a very small price to pay. And I think this is only way I am going to let my tendonapathy cool off enough to fully heal. I will get past this.
Coach Tina – thank you very much for leading and moderating this forum. I have learned a great deal from you and many of the folks posting. This is a challenging injury, and this forum has done much to get me closer to calling my HHT history, though not there yet.
Hi Mike, thank you so much, and thanks for sharing your experience. It is wonderful that you have improved so much recently, and hopefully you are able to kick it for good and have it as a memory before you know it. Thanks for showing others that you can get through it. Is there anything else we can help you with?
Thanks Tina – All set for now – just need to keep the faith 🙂
I’m an athlete and i was injured last july in my butt. I’m a jumper so i cant jump now. Can you please give me some advice? I just do my Theraphy and stretching and istill the pain is there. When i feel i was better, i go to my exercise but after that, the pain come back. like what happen when i jump in the hurdle, my butt like paralized and i can’t walk straight. please give some hope 🙂
Thank you for this info. this help me a lot. Thank you. 🙂
I think you got your answers then 🙂
I am following up on some prior posts I made related to all of this HHT, Ischial Tuberosity, sitting/butt pain. I had four PRP treatments. They did help as my injury was not healing or going away at all. I stopped running, biking, hiking for many months. I can now run and bike. I still have some flare up when I over do it including my gym work but I can get it to heal. I can sit way more comfortably. I can definitely walk pain free. When I run for now I keep my miles low and not too heavy on hills. I am able to sit on my road bike and ride with relatively no pain. I still do not like sitting on wood chairs for too long. I will slip my hand under my butt for relief if needed. By the way Mikes post above about cutting the cushion is tremendous. Overall, I am pretty happy with the PRP treatments and would recommend them.
Thanks for sharing Caryn, glad you are feeling better!
Had surgery for bilateral high hamstring tendinopathy in Finland this week. Dr.Orava who wrote the original article on HHT in 1988 did the surgery. At 48 hours I was able to walk without crutches and had dinner and a beer in a nice Finnish restaurant. Won’t know for a month or so how well the surgery worked however the Finnish group has by far the greatest experience and success with Dr. Orava’a technique. Many professional athletes including David Beckham have been operated there.
Thanks for sharing Robert, interesting to read, and this may provide some comfort to other readers who would be able to go see him. Please keep us updated with your progress!
Good read. I’ve had this for about two weeks now. Got injured while trying to get back to running after a hamstring strain in the other leg. Muscles were not strong enough, my gait was off, and hence, this pain in the butt…. While the pain in the rear is almost entirely gone, the pain in the pelvis area is still there, especially after doing any core/hamstring work. Haven’t been running for about 4 weeks now. Hoping to run half a marathon in 4 months…
Hello, 4 months should be enough time to come back from your hamstring pain, but it would be best to check with a doctor to hear a professionals opinion on it. If you follow our recommendations in this guide, it should help you rehab the hamstring enough to start your training soon. Best of luck!
Just curious. Has anybody made a recovery from this injuiry? I”ve been dealing with it for 1.5 years now. I was able to run some, but finally it’s time to stop and let it heal. I”ve started doing pilates, kettlebell swing and hamstring exercies. There are days when pain is gone, but then something makes it return.
Hi Dan, we do have some runners who have shared in this discussion, that they have completely recovered, but you have to be very committed to a rehab routine like what we mentioned in this article. Many runners have found the alternative treatments also helped. Hope you found some comfort in this article!
My daughter has had a very sore, ache in her high hamstring since about a year ago. We have gone to physical therapy, and have got it x-rayed but we still aren’t sure what is wrong with her hamstring. We think it might be a fracture in her ischial tuberosity or the hamstring tendinopathy but we are not sure. She is a competitive dancer and is doing some very intense things. She took a break once she started to have the pain, but had to countinue dancing after a while. She recently started to have pain in her other hamstring too. Now she is having problems with both hamstrings.
Hi Dani, thanks for sharing. Sorry to hear about your daughter, we would recommend trying the suggestions we gave in this post, and see if any of the other suggestions from other runners helps. Hopefully this helps!
Hi again,
I`ve been trying to get back to running after straining one leg , and having hht (at least that is the current diagnosis.)The problem is that everytime i start developing some momentum doing hamstring/core exercises, i get really sore/ injured.
I was wondering if anybody else has been experiencing serious groin/pelvis pain about 3 weeks after hsving hht. Is this a common pain in this injury, or is it likely that something else is messed up? Currently have major soreness/weakness in the area. This is really getting to be quite demoralizing.
Thanks
I am also suffered the same problem.
I am a professional Physiotherapist, due to heavy work i suffered Hamstring tendinopathy injury.
But i am doing frequently many different stretching exercise. But short period of time it will give relief, but the pain radiate more and more to the lumbar region.
I have had this chronic problem for three years only to realise what it is now. Pain in the glute whilst sitting and driving a car. Sciatic nerve pain, hip pain like bursitis, needle like pain when running, pain when I get out bed, fibrous scar tissue pain, and vibration from impacted and a loss elastic energy and bounce.My running has deteriorated from a 33 min 10 kilometre runner to struggling on running 10 kilometres in under 42 minutes due due neuropathic pain. I have bio mechanical issues with right and left hips. Pelvic tilt and strength imbalances.
Icing helps, spas and swimming is best,light resistance stretching helps, most chiros are bad news can aggravate connective tissue when cracking and cause further tendinitis and alignment issues.
I am not a runner but I have had a torn hamstring for 5 months now and afrer 16weeks of physio I am not sure there is much improvement. Some months prior to the tear infotmupmim the night to usent he loo, over balanced and fell backward on the loo, it hurt a lot but I went back to bed and fell asleep. I am 78 years of age and my walking has been affected, I can’t sit for too long and I can’t stand. I am grateful for this thread as I had no idea how long this problem would cause me a nuisance and I am surprised reading this article how long some have suffered the pain. I saw the consultant yesterday after 16 weeks of physio and the suggestion is that i have ultra sound, if they find an infection I will have an injection but if not then i wont get the injection. There is a waiting list but the suggestion is it could be a month with a follow up app in three months time, to see how i am getting on. I had problems getting the MRI so I am not holding MY BREATH.ncannyounpleasemputnme on your mailing list Ann C
Great article per the usual from RunnersConnect! 🙂 12 weeks ago I was doing uphill speedwork, when I felt pain behind my knee/inner thigh area. It was not so terrible I had to stop, so I finished the run. It progressively got worse and I could not run without pain. I took two weeks off running but was able to maintain my strength training 4x/week. Then I started feeling the pain high up in my glutes and midway on my hamstrings. I started seeing a chiropractor, have had sports massages, I foam roll before and after I workout, and supplement with these exercises that are suggested. I also saw a physical therapist who said I could maintain my workouts. I did run/walks for several weeks and built up to 12 miles which I ran 2 weeks ago. Upon suggestion of the PT I did adductor exercises but I think I overdid that and now I feel pain on inner thigh up to the crotch area. I have a marathon in 5 days but I am still feeling pain ( nothing above a 3 on the pain scale though), it is mostly like a deep ache. Does anyone have any insight into running a marathon with a hamstring injury??
What is wrong?
Which is it?
High Hamstring Tendinopathy Injury, or Proximal Hamstring Tendinopathy, or Ischiogluteal Bursitis, or Ischial Tuberosity Avulsion Fracture, or Piriformis Syndrome,…
What do I do about it?
I have read many, many, blogs and articles on the situation I am experiencing with pain in my Hamstring/Ischial Tendon/”sit bone” area and am no closer to figuring out what is going on or how to fix it.
In the beginning.
I started having the problem (pain) over a year ago. It started (or coincided) with a hamstring pull I suffered while playing soccer. After resting the hamstring for a few weeks and doing light test stretching to determine its wellness, I started running to test it further. All seemed to be ok, with one issue I didn’t associate with the hamstring at the time; I was having pain while sitting. The pain was right on the underside of my “sit bone.” Oddly, I had a similar issue on my right leg years early that I would experience during long drives, that pain when away by itself somehow. So, I didn’t connect the pain with the hamstring pull.
Before I started playing soccer again after the hamstring pull, I did some light sprinting to test it out. During my warm up stretching, I did notice that the hamstring I had pulled (left hamstring) was tighter then the right. However, my sprinting was fine. Onto the game: I stretched and warmed up before the soccer game and all was good. I played fine and could sprint at top speed. It was after the game I noticed the pain in my buttocks somewhere.
So the story goes on.
Since the original pull, the left hamstring has always felt tighter then the right, however after a good warm up and some stretching I could play soccer and didn’t seem to have any performance drop during the game. This cycle continued for months, however the sitting pain increased gradually.
About three months ago, I stopped playing soccer in hopes a rest from quick sprinting would heal my pain. I stopped running altogether also for the first two weeks. I then tried a slow run to keep my legs from deteriorating from lack of running. I stretched before the run and notice my hamstring was even tighter then before and the pain was more pronounced under my “sit bone” when I stretched. I went for the run anyhow and for the first time while running the pain from the “sit bone” area was there. I had to stop the run. The pain in the “sit bone” area was enough to worry me. I have also notice the discomfort/tightness in the area of the “sit bone” when walking or taking on longer strides while walking. I can also detect tightness in my hamstrings in different areas seemingly at random when I walk.
Attempts to get better.
Since that last run where I had to stop I have not run since. That was 10 weeks ago.
During the past 10 weeks, I have researched the best I could my symptoms in hopes of finding solutions. I have run into just as many solutions that are the opposite of other solutions. Specifically, half of the solutions call for stretching and half say no stretching. I tried stretching and the pain* right at “sit bone” was significant. It wasn’t the pain you get with a tight muscle but sharper pain, and following stretching the discomfort while sitting was significant.
*Where is the pain? Here is my best description. I have been calling it the “sit bone” area. However, I have tried to pin point it by probing with my fingers and could not get any reaction that gave me an exact location for the pain. It feels like it is at, or very close to, where the hamstring attaches to the ischail tuberosity. Again, I can push all around the area with my finger and it doesn’t cause a painful reaction. While sitting I can feel pain and will reach down and try to find the pain to no avail. I am beginning to think there is a voodoo doll of me somewhere with a needle in its butt.
I abandoned the stretching solutions for my issue as I agreed with the notion that stretching an injured muscle (or tendon) didn’t make sense.
I have been trying the “light” hamstring exercising to promote blood flow in the area. I also have been doing hip and waist exercises and stretching to keep the area limber. I had read about other tendons or muscle in the area can get tight can affect the tension on the hamstring. After 9 weeks of that, I still have the discomfort in the area and can still notice it while walking.
This has become ridiculous. I have never experience something that 9 weeks of rest didn’t make better.
I have read about bursa sacks causing pain in the area and tendonitis and even stress fractures and pelvic tilt issues affecting the hamstring. I have read about how injections can help and how they can make it worse. It would seem there is no tried and true medical solution. Everyone has had their own independent solutions. It is frustrating.
I have been doing most of the exercises on the listed in the article. The one I don’t do are the stretching ones, as those have caused more lasting pain. I have been doing those exercises for 6-7 weeks now, and have notices a very minor decrease in pain and discomfort while sitting. At this rate I would need to do the exercises for 60-70 weeks to get close to 100% pain free. That seems excessively long.
I have not looked into “Extracorporeal Shockwave Therapy” as I cannot find much literature on it and corticosteroid injections
worry me.
Chiropractic Care?
I did see that chiropractic care is referenced in a few articles. I had actually started getting adjustments by my doctor (a DO) for lower back tightness and after a few treatments seemed to notice a decrease in my discomfort and pain. Unfortunately, I don’t have access to that treatment in my current location, as I have been traveling out of the country (US) for the past 12 weeks. Perhaps the comments about pelvic placement, angle, tilt, have a bigger effect on the hamstrings then I realize.
I am writing this in hopes someone can point me in a direction that can lead to a solution.
Matthew
Matthew,
Your experience is very similar to mine. Short story – I do triathlons, play tennis, and have been active all my life. Over the 2015 holiday break, I played a couple days of intense basketball. Afterwards nothing seemed out of the ordinary except my hamstrings were sore. However, shortly thereafter (within a week or so) I notice a dull ache in my left hamstring while running. The pain wasn’t horrible but I felt myself inadvertently modifying my running gait to compensate for the ache. After that I noticed that the same left hamstring ache would appear while I driving or riding in a car (bucket seats). Oddly I didn’t (and don’t currently) feel pain while sitting in my office chair or even a hard park bench. I ONLY feel the ache when my butt is lower than my knees and there’s slight pressure on my hamstrings (like in a car) or when I run or bike up a hill.
Like many on this post, I scoured articles online to better understand diagnosis and treatments. I would think it was one things and then sway to another – High Hamstring Tendinopathy Injury, Proximal Hamstring Tendinopathy, and Ischiogluteal Bursitis, were all injuries I thought I might have over the past 5 months. Ultimately I began to rehab my hamstring via basic stretching, the introduction of eccentric hamstring exercises, AND I stopped running and biking completely. 6 weeks later . . . nothing. Granted, i only felt the dull pain when I was in the car (bought a wedge cushion on Amazon that helped) or when I sprinted up the stairs multiple times (helping a friend move). I was midly stronger, but knew I wasn’t improving either so I took the next step.
I started by seeing a chiropractor to rule out any back or alignment issues. While he couldn’t find anything wrong with my back or alignment, he did notice an extreme difference in tightness between my left and right hamstrings and encouraged gentle stretches. He also confirmed what I was feeling, in that my left hamstring was weaker than my right. Based on his advice, i received a deep tissue massage on my legs to break up hamstring tissue and began using foam rollers. He theorized that I had some micro-tears in the tendon that connects my hamstring to my sit bone and said it would take 3-4 months to heal. He wasn’t sure but thought shockwave therapy might help which I did a couple of times. While interesting, I didn’t notice a difference over time so I stopped.
I left and re-committed to stretching and strengthening. I continued reading anything I could find online which eventually lead me to believe I had bursitis (because of the pain when my hamstring are not parallel with my butt). My eccentric exercises made both my hamstrings stronger, but alas I never felt like the dull pain was subsiding. Stronger? Yes! Less pain? No . . . not really.
3 months in I decided to bite the bullet and see a sports Orthopedist. He did an x-ray which didn’t show anything and then requested an MRI. The results were pretty anti-climatic. He confirmed that I had tendinitis and prescribed some expensive anti-inflammatory cream that has done nothing to improve my condition. I did ask him about steroid shots and he said that he didn’t recommend it because of the chance of infection. Basically he send my home with $200 cream and a confirmed diagnosis. After spending around $1000 on trying to figure this out, and getting no better, I was completely deflated. I didn’t do anything for a couple weeks wallowing in my defeatist attitude. But alas, seeing people out of their road bikes, and watching people jog around the neighborhood made me re-commit again.
5 weeks later I am still conflicted as to whether stretching helps or hurts. I personally believe stretching helps but it most be done moderately and multiple times a day. I have a couple physical therapy friends who have encouraged me to roll my injured hamstring around on a lacrosse ball to promote blood flow to the injured area (of course NOT on ischial tuberosity). I’ve also read some journals that recommend working the injured area until one experiences a little pain in the sit bone while others claim any pain in that area is bad.
In the past week or so I have noticed that my pain isn’t as bad riding in my car – even after ditching my wedge cushion. Even after playing ultimate frisbee this week (honestly the first time I’ve ran in a couple almost three months) my left sit bone was a little sore but not as bad as I thought it was going to be. Could I be healing or am I fooling myself? That’s the problem. You can’t really tell what’s up vs. down.
Here’s what I “think” is working . . . I have begun sitting on a ice gel pack a couple of times a day (especially after work outs). I am continuing to stretch, but not aggressively and more often – throughout day. I am focused on eccentric hamstring exercises along with planks, elliptical and want to begin swimming and fast walking in pool. I am also on my bike trainer – to keep me flat.
It’s terribly frustrating, BUT being active is part of my life so the search continues! Hope this helps someone out there in the hunt. Send help if you can!
Lance
Have u found any solutions ? Cause I got the same situation as you , same way , same about a year with it , and same sport
Hi there,
I’m looking for some advice on how to manage my High Hamstring Tendonopathy. It’s been 3 months and I still can’t run. I tried a 1 mile jog 2 weeks ago and while I felt no pain during the jog, my leg didn’t feel right and 2 days later the pain in the tendon was much more pronounced. I did have this in both legs, but thankfully my left leg has healed. No pain, no discomfort. My right leg has it very badly. I’ve been doing exercises when I can, and while my pain level has almost disappeared, I’m frustrated that if I try to run 20 feet at normal pace, the pain rears up. Seriously, how long does this stupid thing take to heal? I can’t run, I’m gaining a bit of weight, I’ve committed to doing the exercises I’ve found online, glute bridges, single and double, clam, planks, I use ankle weights on the clams now, I put my feet up on the bed and do single leg lift (kinda like a bridge) from there too. I do single leg lift, but there’s pain with that, so I’m not sure if I’m to do those or not? Any advice anyone here can give, will be greatly appreciated. I also try to walk at least 2-3 miles 2-3 times a week. It’s driving me batty because I wish to run so much!! What else can I do and how much longer is this going to take??
Massively frustrated,
Minnesota Runner
Hello,
I have been dealing with a similar injury in the hamstring for about 6 months, except instead of the proximal side of the hamstring, the pain is on inside and behind the knee where the semitendinosus connects to the tibia (pes anserine area). Although expensive, ART, Graston and Shockwave helped when the pain was worse, but I can’t shake it and it still threatens to return if I increase mileage or speed.
My question is, are the treatments offered in this article (eccentric, stretching, etc.) the same advice for to lower hamstring tendonitis injuries as well? Or, are there different stretches or advice?
Thanks for your help.
KD
good presentation about hamstring …..thank for runners connect
I have probably had this injury for at least 10 years. Sitting pain on the left was my marker. I did PT of all kinds before seeing a hip specialist, who diagnosed me with hip dysplasia. Apparently I’d had that for years and consequently, torn labrums on both side, FAI, CAM, you name it. Hips torn up. I spent 5 years going through major surgeries. Hip scopes to repair all the tears and even replace my left labrum. Hip preservation surgery to correct the dysplasia and prevent need for early replacement on both sides. One revision surgery on the right because my pelvis didn’t fuse back together. That one involved a screw through the bottom of the pelvis. That screw did not stay all the way in and sat in my right hamstring tendon for a year before it could be removed. With all of that done, my sitting pain on the left remained. I sat on ice at work all day. I did graston and ART (the only things that helped some, though didn’t rid me of the injury). Turns out, as I had been saying for years, the sitting pain was not from hips or back issues. My 7th surgery, at the end of 2017, was to go look at that hamstring tendon. My surgeon found a partial tear at the ischial tuberosity and a ton of scar tissue. He debrided the scar tissue, took the tendon off the bone, and reattached it.
I am recovered from all surgeries and running again. However I believe I have tendinopathy in both hamstring tendons now. I have done 3 sets of PRP injections on each side. It seemed to help some but definitely still have issues. I run because I love it and it makes me feel like me. I am running 2-3 times a week, usually 3 miles at a time, plus elliptical a day or two a week. I ran 4.3 miles yesterday and enjoyed it, even though I have pretty intense soreness at the ischial tuberosity end of the tendons. I have toddlers so I cannot do all the training I would like, but I do try to keep up core strength with planks and side planks 3-4 times a week, push ups, bridges when I can (not as consistent as I should be), squats when I can, weightlifting occasionally. I am 46 and female. I am trying to accept that this is just where I am and I will have pain when I sit or work out.
Thank you for this presentation. Sorry for the long post, but do you have any advice for my complicated, advanced case?